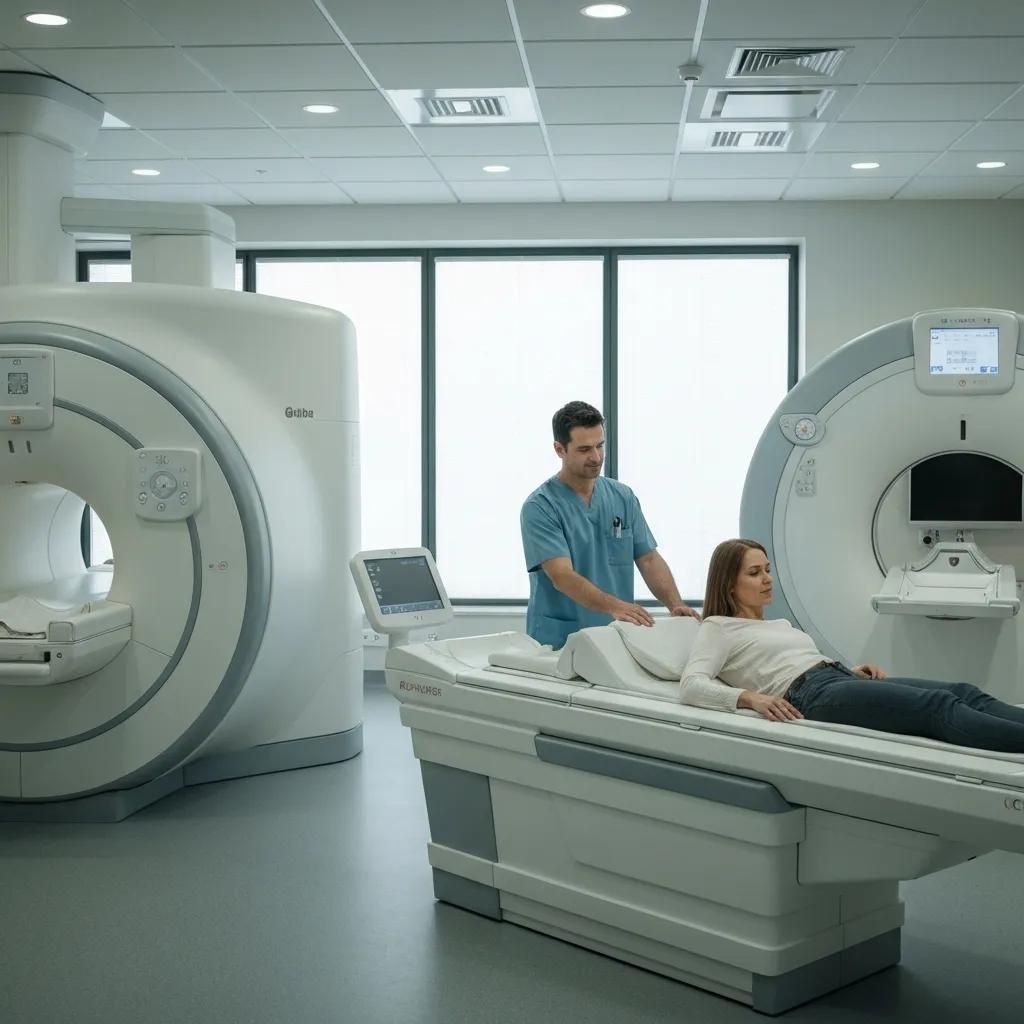
Medical Imaging Services & Booking Guide at Life Medical Imaging
Medical imaging encompasses a range of diagnostic techniques—such as X-ray, ultrasound, CT and MRI—that let clinicians see inside the body to detect disease, plan treatment and support preventative health. These imaging methods work through different mechanisms (ionising radiation, sound waves, magnetic fields), each delivering specific diagnostic value that improves early detection and clinical decision-making. Readers will learn how major modalities work, how to prepare for scans, what to expect for costs and Medicare options, and how patient-centred imaging pathways reduce anxiety and improve outcomes. Many patients worry about safety, preparation or result timelines; this guide answers those concerns in plain language and shows practical steps to make booking or enquiring straightforward. Below you will find clear comparisons of modalities, step-by-step preparation checklists, cost and billing guidance for Australian settings, and descriptions of how modern centres support patients from referral to reporting. After this introduction there is a short, compassionate note explaining how imaging services typically handle bookings and enquiries to make the next steps simple and reassuring.
If you need help booking or enquiring about a scan, imaging centres specialise in clear patient information and easy appointment pathways that prioritise compassionate care and early detection. When contacting a centre, you can ask about available modalities, Medicare or bulk billing options, and any interpreter or accessibility needs; centres generally guide you through referral requirements and preparatory instructions. Centres emphasise patient-centred care and advanced technology to support accurate diagnosis and timely reporting while keeping bookings straightforward and responsive. If you have a referral, bring any previous imaging reports and your referral form to help clinicians coordinate care and reduce repeat imaging.
What Are Medical Imaging Services and How Do They Support Early Detection?
Medical imaging services are diagnostic healthcare procedures that create pictures of internal anatomy to identify disease, monitor treatment and guide interventions. By revealing structural and functional changes before symptoms become severe, imaging supports earlier diagnosis and more targeted treatment, which can improve outcomes and reduce invasive procedures. Imaging also underpins many screening and surveillance programs that catch conditions such as cancer or cardiovascular disease at an earlier, more treatable stage. Understanding how different modalities contribute to early detection helps patients and referrers choose the appropriate test for a specific clinical question, linking the right technology to the right condition.
What Types of Diagnostic Imaging Are Available in Australia?
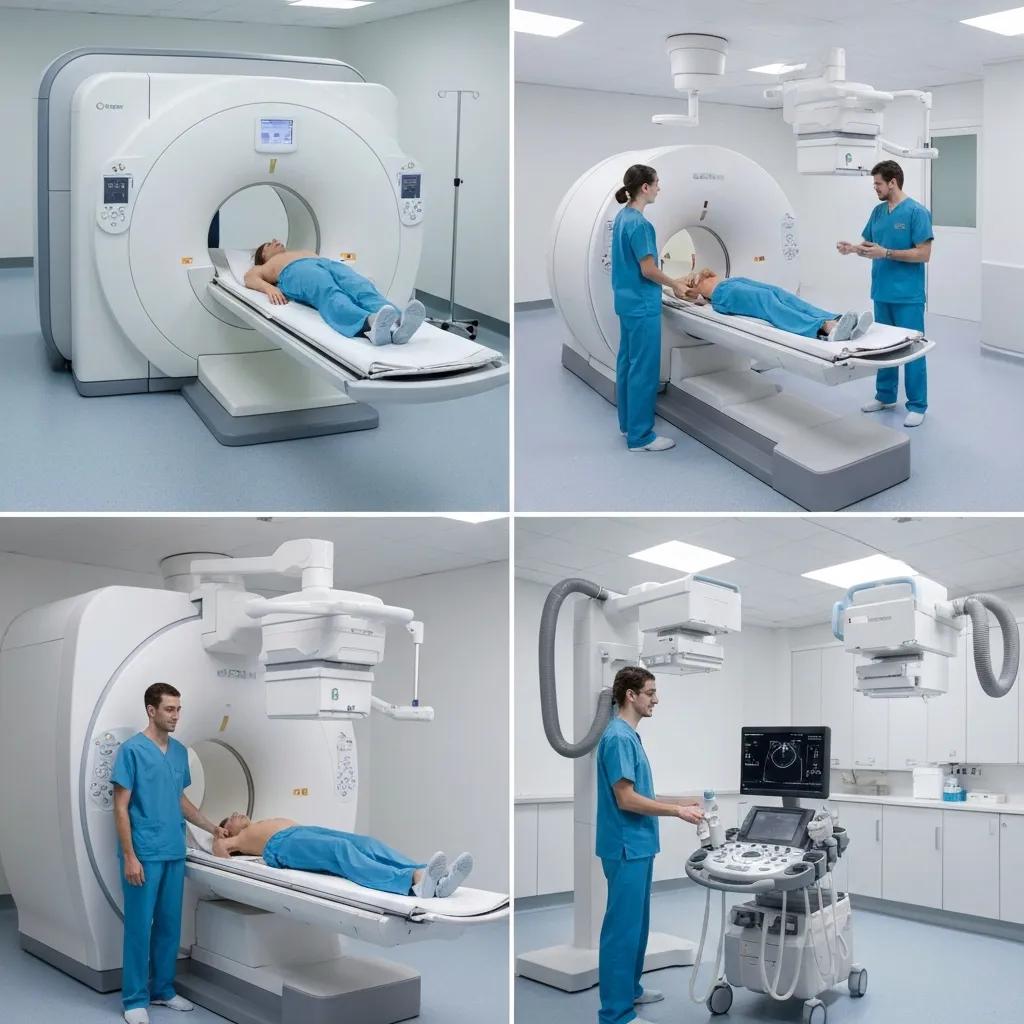
Australia provides a wide range of diagnostic imaging modalities used across public and private settings to match clinical needs and patient circumstances. Each modality has strengths tailored to particular conditions and body regions, and availability may vary by region and facility type. The most common options include MRI for soft tissue detail, CT for rapid cross-sectional images, ultrasound for real-time examinations without radiation, and X-ray for bone and chest assessments. Other specialised services include mammography for breast screening, DEXA for bone density, nuclear medicine/PET for functional imaging, interventional radiology for image-guided procedures, and dental imaging (OPG/CBCT) for oral health planning.
- MRI Scan: Offers high soft-tissue contrast for brain, spine and joint assessment and is ideal when detailed tissue characterisation is needed.
- CT Scan: Delivers rapid cross-sectional images suitable for trauma, chest and abdominal assessment and for detecting acute pathology.
- Ultrasound Imaging: Uses sound waves for real-time imaging of pregnancy, abdominal organs and musculoskeletal structures without ionising radiation.
- X-ray Services: Provides quick, low-cost imaging for fractures, chest disease and skeletal evaluations.
- Mammography: Specialised X-ray optimised for breast tissue screening and diagnostic assessment.
- DEXA (Bone Densitometry): Measures bone mineral density to evaluate osteoporosis risk.
These modality descriptions lead naturally to a closer look at the mechanisms behind each major scan and why clinicians choose one over another.
How Does Early Detection Improve Patient Outcomes Through Imaging?
Early detection through imaging shortens the time to diagnosis, enabling clinicians to begin targeted treatment sooner and often with less invasive options. For example, identifying small cancers or early cardiovascular changes allows for earlier interventions that improve survival rates and reduce long-term morbidity. Imaging also monitors disease progression and treatment response, which optimises therapy choices and can prevent unnecessary procedures. Public health screening programs and surveillance imaging target high-risk groups to catch disease before symptoms arise, and coordinated imaging pathways help translate early findings into timely clinical action.
- Early detection reduces downstream treatment complexity and can preserve function.
- Surveillance imaging informs personalised care plans and helps avoid overtreatment.
- Rapid, accurate imaging supports multidisciplinary teams in making evidence-based decisions.
This understanding of outcome benefits sets up a practical comparison of how MRI, CT, ultrasound and X-ray actually produce images and when each is preferred.
How Do MRI, CT, Ultrasound, and X-ray Scans Work?
MRI, CT, ultrasound and X-ray rely on different physical principles to create diagnostic images, and choosing between them depends on the clinical question and patient factors. MRI uses magnetic fields and radiofrequency pulses to map soft tissue contrast without ionising radiation, making it ideal for brain, spine and joint imaging. CT utilises ionising X-rays in a rotating gantry to capture rapid cross-sectional images with excellent spatial resolution for trauma and chest/abdominal assessment. Ultrasound sends and receives high-frequency sound waves for real-time imaging, widely used in obstetrics and abdominal imaging. Plain X-ray delivers a fast, low-dose snapshot optimal for bone, chest and dental screening.
Before the comparison table, a concise summary helps readers choose modalities by mechanism and typical uses. The table below compares common modalities in a quick reference format suitable for patients and referrers.
This comparison clarifies modality selection and leads into deeper MRI-specific considerations and procedural expectations for CT and ultrasound.
What Should You Know About MRI Scans and Their Uses?
MRI scans are non-ionising and provide exceptional soft-tissue contrast, which makes them invaluable for diagnosing neurological conditions, spinal disorders and many joint injuries. Safety considerations include screening for some metal implants or devices, as the strong magnetic field can interact with ferromagnetic materials, so telling staff about implants is essential. Some MRI examinations use contrast agents to improve lesion detection; staff will review allergies and kidney function when contrast is planned. Claustrophobia and noise are common patient concerns, and centres typically offer strategies such as shorter bore machines, ear protection, calming communication and, when needed, pre-scan anxiolytic pathways.
Patients who understand these issues are more likely to have a calm and successful scan, and knowing about implant screening or contrast consent helps clinics plan the safest, most effective examination. The next section describes what to expect for CT scans and ultrasound procedures.
How Are CT Scans and Ultrasounds Performed and Prepared For?
CT scans are usually rapid and performed with the patient lying on a motorised table that moves through the scanner while X-rays rotate to collect data; some studies require an intravenous contrast injection and breath-hold cooperation. Contrast improves visibility of blood vessels and enhances tissue contrast, but staff screen for allergies and kidney function before administration. Ultrasound is operator-dependent and involves applying gel and moving a transducer over the skin to capture real-time images; certain ultrasound exams require fasting or a full bladder for optimal visualisation. Both CT and ultrasound procedures are typically explained on arrival, with staff supporting positioning, safety checks and answering patient questions to reduce anxiety.
Preparation and clear communication around contrast and fasting are vital to obtaining diagnostic-quality images, which in turn supports accurate clinical decisions and faster care pathways.
How Can Patients Prepare for Common Imaging Procedures Like CT Scans and MRIs?
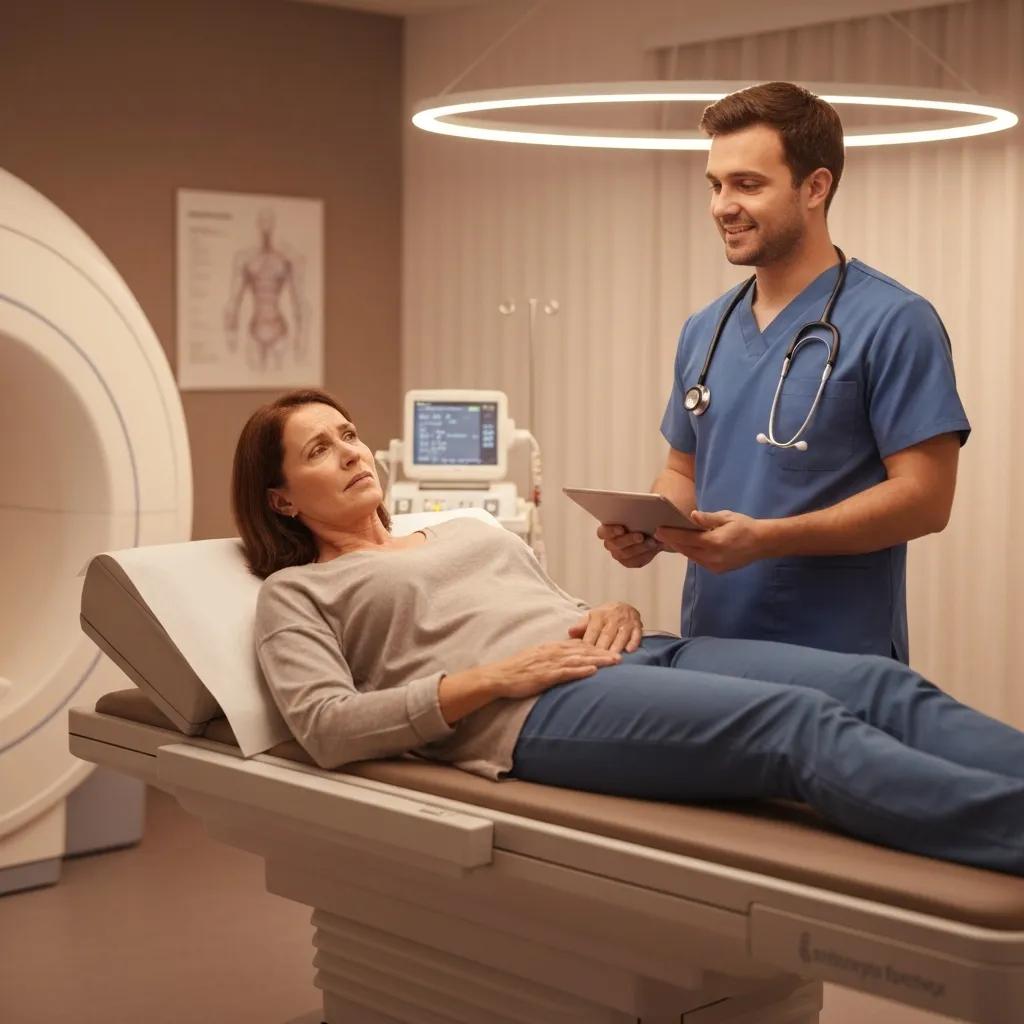
Preparing correctly for imaging reduces delays, improves diagnostic quality and minimises the need for repeat scans. Key pre-appointment actions include confirming the referral, checking whether contrast is required, arranging transport if sedation is planned, and bringing previous imaging or relevant medical records. Clothing and metal removal are common steps across modalities, and patients should follow fasting or hydration instructions specific to the procedure. Clear explanations of consent, potential contrast reactions and expected timelines help patients give informed permission and arrive ready for their appointment.
Below is a focused preparation checklist for CT and MRI appointments to guide patients through essential steps that clinics commonly request.
What Are the Key Preparation Steps for CT Scan and MRI Appointments?
Patients scheduled for CT or MRI should complete a few simple steps to ensure the scan proceeds safely and produces usable diagnostic images. First, review and bring the referral and any previous imaging reports to avoid repeat exposure and to help interpreting clinicians. Second, disclose allergies, medications, pregnancy status and any implanted devices during pre-screening so staff can assess contrast safety and magnetic compatibility. Third, follow fasting or hydration instructions when contrast is planned and arrange transport home if sedation or anxiolytics may be used.
These steps reduce last-minute cancellations and enable staff to focus on patient safety and image quality, setting the stage for clear reporting and clinical decision-making.
Are There Special Considerations for Ultrasound and X-ray Preparations?
Ultrasound and X-ray generally require less preparation but have important exceptions that patients should know before arriving. For abdominal ultrasound, fasting for 4-6 hours often reduces bowel gas and improves visualisation, whereas pelvic ultrasound commonly asks for a full bladder to displace bowel and provide an acoustic window. X-rays usually have no special prep, but pregnancy status must be disclosed so staff can take protective measures or choose alternative imaging. Paediatric imaging often involves distraction, comfort measures and sometimes parental presence to reduce distress and improve cooperation.
Understanding these exceptions helps patients comply with instructions and ensures clinicians obtain the right diagnostic information at the first visit.
What Are the Costs and Medicare Options for Medical Imaging in Australia?
Costs for medical imaging vary by modality, facility type (public vs private), urban or regional location, and whether Medicare rebates or bulk billing apply for specific services. Medicare commonly rebates a portion of diagnostic imaging when a valid referral from an authorised provider is present, but out-of-pocket costs may apply for private clinic services, specialist protocols or contrast-enhanced studies. Bulk billing availability differs between centres and regions; some major metropolitan services offer bulk billing for selected scans, while other clinics may charge a fee with a partial Medicare rebate. Knowing your referral entitlements and asking clinics about bulk billing or concession eligibility before booking helps manage expectations and plan for any out-of-pocket costs.
Practical steps to enquire or book an appointment are outlined below to make the billing and booking process straightforward for patients.
- Confirm you have a valid referral from an authorised referring clinician before contacting a centre.
- Ask the centre whether the requested study is bulk billed, partially rebated by Medicare, or will incur an out-of-pocket fee.
- Bring your Medicare card, referral form, and any prior imaging reports to the appointment to facilitate billing and comparison.
By following these steps you can clarify costs ahead of time, which reduces unexpected charges and supports timely access to needed imaging.
How Does Bulk Billing Work for Radiology Services in Melbourne and Sydney?
Bulk billing means the clinic accepts the Medicare benefit as full payment for a service and charges no out-of-pocket fee to the patient, but its availability varies by region and provider policies. In large metropolitan areas like Melbourne and Sydney, some public and private clinics offer bulk billing for specific, eligible diagnostic tests or for patients who meet concession criteria, whereas other providers may charge an account fee with a Medicare rebate. To confirm bulk billing availability, patients should ask when booking, present their Medicare details and referral, and clarify whether any specialised protocols or contrast use might attract additional charges.
Checking bulk billing options at booking helps patients plan and prevents surprises, and it also supports informed decisions about attending private versus public imaging services.
What Are Typical MRI Scan Costs in Sydney and Other Regions?
MRI costs depend on the type of study, use of contrast agents, whether a specialist technique is required, and the clinic’s billing model; public hospital imaging may be covered for admitted patients or through scheduled outpatient services, whereas private clinics often involve out-of-pocket fees that vary by region. Medicare rebates can offset part of private fees when a valid referral exists, but the core drivers of cost include scan complexity, anaesthetic or sedation needs, and reporting urgency. Patients travelling from regional areas may encounter additional access-related expenses, so discussing transport support or regional referral pathways with both the referrer and imaging centre can help manage logistics.
Transparent discussion about expected costs when booking ensures patients understand rebate entitlements and any likely out-of-pocket components before attending.
How Do Care Imaging Centres Ensure Patient-Centred Radiology Services?
Care imaging centres design processes around clear communication, compassionate care and easy booking pathways to reduce patient anxiety and improve diagnostic efficiency. Patient-centred measures typically include accessible pre-appointment information, straightforward referral confirmation, clear consent and contrast screening procedures, and staff trained to support patients with claustrophobia, language needs or mobility limitations. Centres also invest in advanced imaging technology and workflow enhancements—such as AI-assisted prioritisation and teleradiology reporting—to shorten turnaround times and maintain diagnostic accuracy for both metropolitan and regional patients. These systems help clinicians get timely, reliable reports and help patients feel informed and supported throughout the imaging journey.
- Clear pre-appointment instructions reduce no-shows and improve scan quality.
- Flexible appointment scheduling and communication options support diverse patient needs.
- Staff education in communication and comfort measures eases anxiety for vulnerable patients.
Explaining technologies and team roles next clarifies how these patient-centred benefits are delivered.
What Technologies and Expertise Are Used in Modern Medical Imaging?
Modern imaging combines high-field MRI and low-dose CT hardware with digital radiography, sophisticated software and emerging AI tools to improve image quality, reduce radiation exposure and speed reporting workflows. AI-assisted algorithms can flag urgent cases, enhance detection of subtle findings and streamline administrative tasks, while teleradiology enables specialist reporting for regional clinics that lack on-site subspecialists. Dose-reduction technology and iterative reconstruction in CT help minimise ionising exposure without sacrificing diagnostic detail, contributing directly to patient safety and long-term risk management. These advances increase diagnostic confidence and make imaging more accessible across diverse practice settings.
Understanding these technologies clarifies how staff roles complement hardware and software to produce accurate, timely reports for referrers and patients.
How Do Radiologists and Sonographers Support Your Imaging Journey?
Radiologists are medical specialists who interpret imaging studies and produce clinical reports that guide diagnosis and management, while sonographers and radiographers perform the examinations and ensure high-quality image acquisition. The imaging team communicates with referring clinicians to clarify clinical questions, recommend further targeted imaging when needed, and prioritise urgent findings for rapid action. Sonographers and radiographers also provide patient-focused explanations and comfort measures during the scan, and radiologists review images, integrate clinical history, and generate structured reports for the referrer. This multidisciplinary interaction ensures that imaging contributes meaningfully to patient care at each step.
Knowing who does what helps patients anticipate the process and feel confident about the clinical steps that follow imaging.
What Are the Most Common Patient Questions About Medical Imaging?
Patients frequently ask about safety, radiation exposure, contrast reactions, claustrophobia and how soon they will receive results; clear, evidence-based answers reduce anxiety and support informed consent. Imaging safety follows principles of minimising radiation exposure and screening for contrast or implant-related risks, with alternative modalities available when appropriate. Result timelines vary by study urgency and clinic workflows, but centres aim to deliver timely reports to referring clinicians and to help patients understand next steps for follow-up or treatment. Below are concise, practical answers to these ongoing concerns to help patients know what to expect.
Is Diagnostic Imaging Safe and What Are the Risks?
Diagnostic imaging is generally safe when performed with appropriate indications, radiation dose optimisation and pre-screening for contrast safety; for MRI, the main safety considerations are metal implants and patient tolerance of the magnetic environment. Radiation exposure from a single X-ray or CT scan is usually low relative to natural background exposure, and modern CT protocols emphasise low-dose techniques to keep exposure as low as reasonably achievable. Contrast agents have well-established benefit-risk profiles; screening for prior reactions, renal function and relevant medications reduces the risk of adverse events. Patients should discuss individual risks with referrers so that the chosen modality balances diagnostic benefit and safety.
Reducing risk often means choosing the most appropriate modality for the clinical need and communicating medical history fully before the scan.
How and When Will I Receive My Imaging Results?
Reporting timelines depend on urgency and the modality: urgent or inpatient studies are prioritised for immediate reporting, while routine outpatient studies commonly return reports within 1 to 5 business days. The typical pathway is that the radiologist generates a report which is sent to the referring clinician, who then discusses results and next steps with the patient; some centres also provide direct patient copies on request. If results are time-sensitive, imaging centres and referrers coordinate to ensure rapid communication and follow-up. If you have not heard back within the expected timeframe, contact your referring clinician to check the report status and any recommended actions.
Knowing this pathway helps patients understand when and how they will be informed, and prepares them to follow up if necessary.
If you would like to book an appointment or enquire about a specific scan, most imaging centres make booking and enquiries straightforward: confirm your referral, ask about Medicare or bulk billing options, and request any special support you need such as interpreter services or anxiety management. When booking, have your referral, Medicare details and prior imaging reports available to speed the process and help staff advise on preparation steps. Centres that emphasise patient-centred care will guide you through contrast screening, arrival timing and comfort measures so the appointment meets both clinical and personal needs. Taking these simple administrative steps before your visit helps the clinical team focus on delivering timely, accurate imaging and clear next steps for your health.