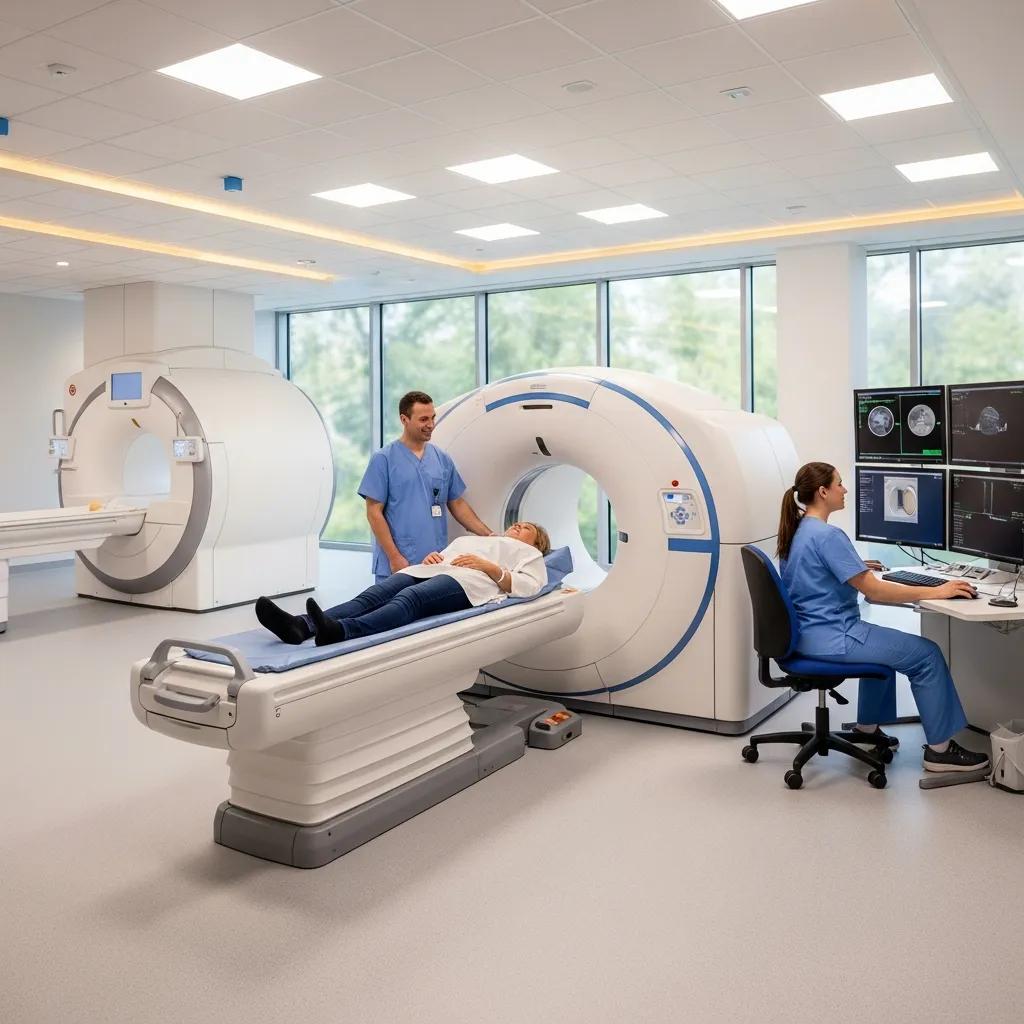
Comprehensive radiology and medical imaging services at Life Medical Imaging Central Coast
Medical imaging—often called radiology—combines specialised equipment with expert interpretation to diagnose illness, guide treatment and monitor recovery across many clinical settings. This guide walks through the main imaging options—CT, MRI, ultrasound, X‑ray and bone densitometry—explaining how each works, what it best assesses, and practical steps patients and referrers should take before and after a scan. Clinicians and patients frequently need clear direction on which test suits a given symptom, how safety and dose are managed, and which technological advances are enhancing diagnostic accuracy in 2024. We address those questions with modality-by-modality explanations, concise preparation checklists, safety comparisons and a look at emerging trends such as AI-assisted reporting and photon-counting CT. Throughout, you’ll find practical advice for common referral scenarios, patient preparation tips and examples of how a NATA‑accredited independent provider applies low-dose techniques and specialist services to improve care on the Central Coast.
What medical imaging services does Life Medical Imaging Central Coast offer?
Medical imaging includes several modalities, each using different physics to visualise anatomy and disease. Each test brings unique diagnostic value by emphasising contrast, resolution or functional detail. CT uses X‑rays and reconstruction algorithms to produce fast cross‑sectional images ideal for bone detail, acute trauma and vascular assessment. MRI uses magnetic fields and radiofrequency signals to give excellent soft‑tissue contrast for neurological and musculoskeletal problems. Ultrasound delivers real‑time, radiation‑free imaging suited to obstetric, gynaecological, vascular and musculoskeletal assessment. Digital X‑ray and dental imaging remain quick, cost‑effective first‑line tools for skeletal and dental concerns. Bone mineral densitometry (DEXA) measures bone density to assess osteoporosis risk, and interventional image‑guided procedures—including PRP injections—support both diagnosis and therapy. Knowing these differences helps clinicians choose the right test and helps patients understand what each study will show.
Medical imaging modalities: their role in diagnosis, treatment and monitoring
Medical imaging plays a central role in modern healthcare by enabling non‑invasive visualisation of internal structures for diagnosis, treatment planning and follow‑up. Modalities such as X‑ray, PET, CT, MRI and ultrasound each contribute different strengths. Advances in medical image processing have improved detection and characterisation of disease, and are increasingly used alongside machine learning and deep learning to support clinical decision making. While automated tools can enhance workflow and flag findings, human oversight remains essential to ensure accuracy and clinical relevance. This review summarises working principles, clinical benefits and limitations across modalities and highlights recent methodological developments and future directions in the field.
Recent trend in medical imaging modalities and their applications in disease diagnosis: a review, B Abhisheka, 2024
Life Medical Imaging Central Coast provides these services across multiple Central Coast locations, including ultra‑low dose CT and dedicated women’s and cardiac imaging pathways as part of our clinical capability. The list below summarises core services and common indications to help referrers and patients select the most appropriate modality.
- CT and ultra‑low dose CT: rapid assessment for trauma, pulmonary and vascular conditions.
- MRI: detailed soft‑tissue characterisation for brain, spine and joint pathology.
- Ultrasound: obstetric monitoring, vascular studies, musculoskeletal and general abdominal imaging.
- Digital X‑ray and dental imaging: fast screening for orthopaedic, chest and dental concerns.
- Bone mineral densitometry (DEXA): quantitative bone density and body composition analysis.
- Interventional procedures: image‑guided injections, biopsies, aspirations and PRP therapy.
This concise service list shows the clinical breadth available and provides a quick reference for common referrals. For booking or referral guidance, clinicians and patients can contact Life Medical Imaging Central Coast through our published enquiry channels to arrange appointments or discuss the most suitable test.
This table highlights each modality’s strengths and links test choice to clinical need. The next section explains CT subtypes and their specific roles.
Which types of CT scans are available and what are their uses?
CT includes several subtypes tailored to clinical questions. General CT produces rapid axial slices for broad evaluation. Cardiac CT (including CT angiography) visualises coronary and vascular anatomy, while angiographic CT focuses on contrast‑enhanced vessel mapping for aneurysm or stenosis. Ultra‑low dose CT uses optimised acquisition and iterative reconstruction to substantially reduce radiation while preserving diagnostic quality for many indications—such as lung nodule follow‑up and routine trauma imaging. CT’s speed and spatial resolution make it the test of choice for acute bleeding, complex fractures and vascular emergencies where rapid diagnosis changes management. Choosing the right CT subtype helps balance diagnostic yield against radiation exposure and allows protocol selection to match the clinical question.
This discussion of CT dose and mitigation naturally leads into MRI’s complementary strengths, especially when radiation avoidance and soft‑tissue characterisation are priorities.
How do MRI scans benefit diagnosis and treatment?
MRI delivers exceptional soft‑tissue contrast, giving detailed views of the brain, spinal cord, intervertebral discs, ligaments and intra‑articular structures—making it especially valuable for neurological conditions, degenerative spine disease and complex joint problems. MRI can characterise tissue composition, detect inflammation and help distinguish tumours from non‑neoplastic lesions, informing surgical planning, targeted therapy and long‑term management. Specialised sequences (for example diffusion and perfusion) and contrast agents extend MRI’s diagnostic reach in oncology and stroke care. Because MRI does not use ionising radiation, it is preferred for serial monitoring, paediatric imaging and situations where cumulative dose is a concern.
How does ultrasound diagnostic imaging support patient care?
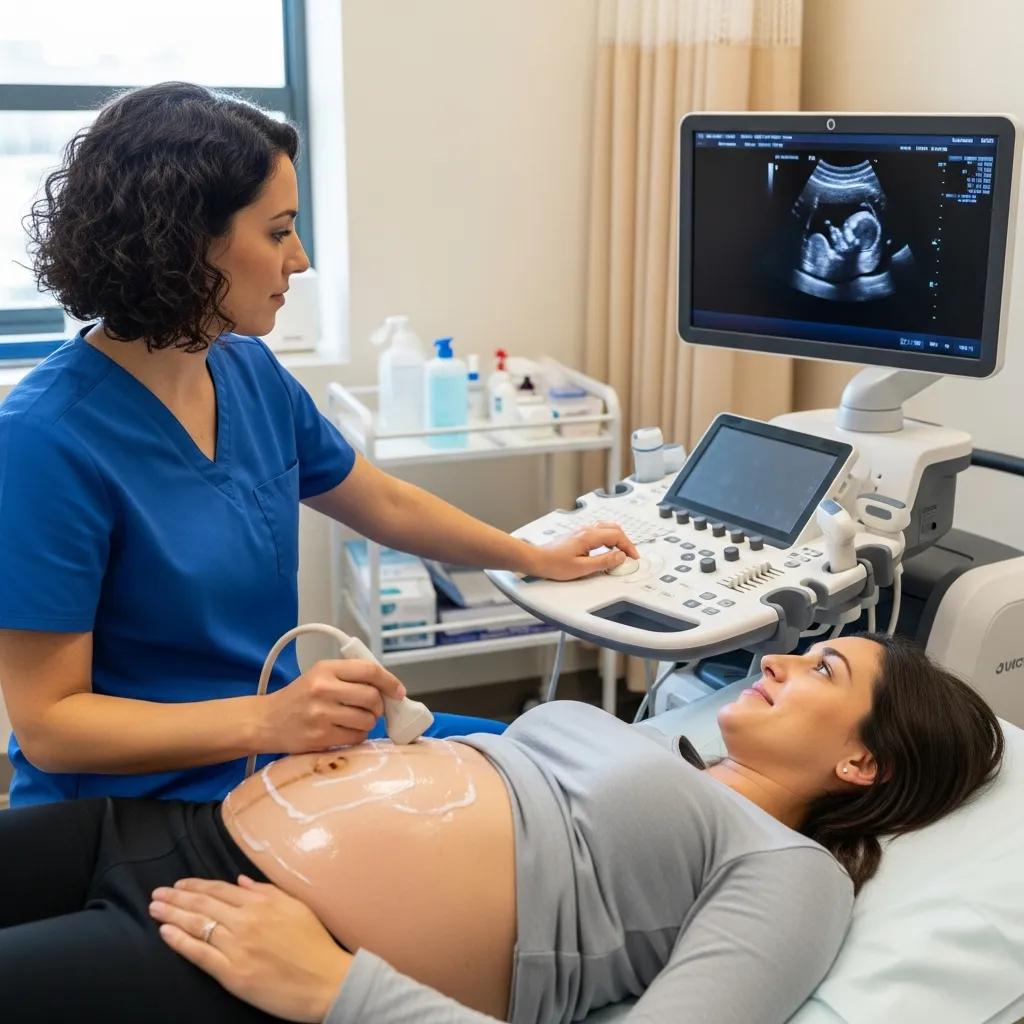
Ultrasound uses high‑frequency sound waves from a probe to produce real‑time images and Doppler assessments of blood flow, offering radiation‑free evaluation for both diagnosis and image‑guided treatment. It excels where dynamic assessment aids diagnosis—observing tendon movement under load, performing compression tests for DVT, or guiding needles during injections and aspirations. Ultrasound’s portability and immediacy let clinicians correlate findings with the clinical exam at point of care and support fast triage decisions in outpatient and emergency settings. Its safety and versatility make it indispensable for obstetric monitoring, vascular assessment and musculoskeletal care.
Our specialised women’s imaging services are closely aligned with obstetric and gynaecological ultrasound requirements, supporting pregnancy monitoring, pelvic imaging and clear referral pathways for patients and clinicians.
- Real‑time assessment of foetal viability and growth.
- Vascular duplex studies for DVT and carotid flow assessment.
- Musculoskeletal dynamic scans for tendon and joint pathologies.
These practical applications show how ultrasound complements clinical diagnosis and workflow. The next subsection outlines obstetric and gynaecological scan types and timing.
What are the key applications of obstetric and gynaecological ultrasound?
Obstetric ultrasound provides time‑staged assessments including early pregnancy viability and dating scans, mid‑trimester morphology/anatomy checks, and later scans for growth, placental position and Doppler assessment of foetal‑maternal circulation. Gynaecological ultrasound evaluates uterine and ovarian structure, identifies masses or cysts, and assists fertility assessment and procedural planning using transvaginal or transabdominal approaches as required. These scans guide prenatal care, detect findings that may alter obstetric management and support timely referral to specialists. For many patients, regular ultrasound monitoring reduces uncertainty, tracks response to treatment and supports joint decision making between clinicians and families.
How does musculoskeletal and vascular ultrasound aid diagnosis?
Musculoskeletal (MSK) ultrasound visualises tendons, ligaments, bursae and superficial joints with dynamic imaging that can reproduce symptoms during the scan—improving sensitivity for tears, enthesopathy and inflammatory change. Vascular duplex combines structural imaging with Doppler flow assessment to diagnose DVT, carotid stenosis and peripheral arterial disease non‑invasively, and serial duplex studies monitor treatment response. Ultrasound also supports image‑guided procedures—tendon sheath injections, joint aspirations and percutaneous bursal treatments—improving accuracy and reducing complication rates compared with blind techniques. The dynamic and interventional strengths of ultrasound lead naturally into safety considerations for all modalities, which we address next.
What are the benefits and safety considerations of radiology procedures?
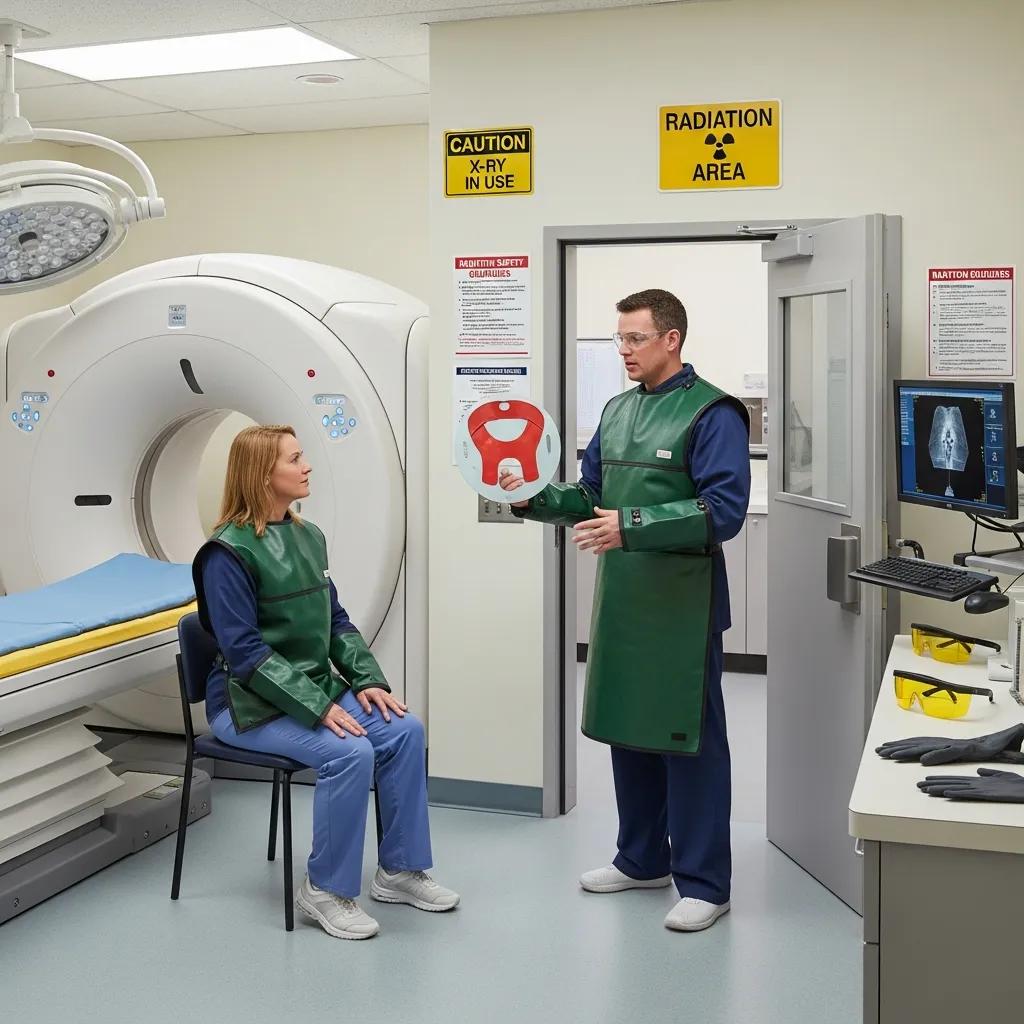
Radiology enables earlier diagnosis, targeted treatment planning and minimally invasive therapeutic options, but each modality brings specific safety considerations that must be weighed against clinical benefit. CT and X‑ray use ionising radiation and therefore require dose optimisation; MRI avoids radiation but needs careful screening for implants and considered use of contrast; ultrasound is radiation‑free but relies on operator skill and exposure guidelines—particularly in foetal imaging. Contemporary practice follows ALARA (as low as reasonably achievable) principles, uses paediatric‑specific protocols and demands evidence‑based justification for imaging choices to minimise unnecessary exposure while preserving diagnostic accuracy. The table below summarises common modality‑specific safety concerns and standard mitigation strategies to guide clinicians and reassure patients.
That summary clarifies risks and common mitigations. The next subsection explains why reducing CT radiation dose matters and how we approach it clinically.
Why is low radiation dose important in CT scans?
Reducing radiation dose in CT matters because ionising radiation carries a stochastic risk that rises with cumulative exposure. Many patients undergo repeated imaging for chronic conditions or cancer surveillance. Low‑dose techniques—such as automated exposure control, iterative reconstruction and protocol tailoring—lower effective dose while keeping diagnostic detail for many indications. Ultra‑low dose CT broadens safe options for follow‑up of stable conditions and lung screening. Clinical justification remains essential: when CT will change management, the diagnostic benefit usually outweighs small radiation risks; where MRI or ultrasound provide sufficient information, those alternatives should be considered to limit exposure. This risk–benefit approach informs patient preparation and modality selection.
How safe is ultrasound imaging for pregnant women and children?
Ultrasound is considered safe for pregnant women and children because it does not use ionising radiation; this underpins routine obstetric care and paediatric imaging where repeat assessment is common. Standard precautions still apply: sonographers observe ALARA for exposure time and acoustic output, and Doppler is used carefully in early pregnancy to limit thermal effects. Clinical guidelines support ultrasound for most pregnancy indications and for paediatric soft‑tissue or abdominal complaints. Clear explanation of why ultrasound is preferred and what the scan will assess helps reduce anxiety for patients and families.
How can patients prepare for radiology and medical imaging appointments?
Good preparation improves image quality, reduces repeat scans and makes the appointment smoother. Preparation varies by modality but commonly includes fasting for some CT/MRI contrast studies, removal of metallic items for MRI, and hydration for vascular tests. Patients should get clear instructions from their referrer or our team about medications, contrast allergy screening and arrival time for administrative and safety checks. On the day, facilities usually complete safety questionnaires, pregnancy screening where relevant and obtain consent for contrast or interventional procedures. Knowing typical wait times and scan durations helps patients plan transport and support. The quick reference table below summarises common preparation steps and expected timeframes to help patients and referrers plan.
Patients who need to book or discuss specific preparation steps can contact Life Medical Imaging Central Coast via our public enquiry channels—our staff will provide modality‑specific instructions and appointment guidance tailored to clinical needs.
- Follow fasting and hydration instructions for contrast or abdominal imaging.
- Bring medication details and allergy history to your appointment.
- Bring identification and referral paperwork as required by the imaging facility.
This table provides a practical preparation checklist and time expectations. The next subsection outlines typical in‑scan experiences and tips to manage anxiety.
What should patients expect during CT, MRI and ultrasound scans?
CT scans are usually brief and quiet: you lie on a motorised table that moves through the gantry and you may be asked to hold your breath for clear thoracic or abdominal images. MRI exams take longer and can be noisy due to gradient switching; you’ll be positioned in the bore, offered ear protection and should tell staff about implants or claustrophobia so comfort measures or sedation can be arranged if needed. Ultrasound involves direct contact with a transducer and gel, and allows real‑time interaction with the sonographer—sometimes reproducing symptoms during dynamic manoeuvres. Clear explanations before and during the scan reduce anxiety and improve cooperation, which enhances image quality and helps clinic flow.
After your scan, patients and clinicians commonly want timely access to reports and images. The following subsection explains report turnaround and how results are shared.
How can patients access and understand their imaging results?
Radiologists prepare imaging reports that are returned to the referring clinician within agreed turnaround times that vary by urgency and modality. Urgent or critical findings are communicated immediately to the referrer to expedite care; routine reports follow standard reporting windows. Patients typically receive results through their referring clinician, who interprets the imaging in the wider clinical context and outlines next steps. Imaging providers can supply copies of reports and images on request or advise how to discuss results with the referrer. Knowing the structure of a radiology report—clinical history, technique, findings and impression—helps patients focus on the key, actionable points. If clarification is needed, a direct conversation with the referrer or radiologist can explain implications for treatment and follow‑up.
What are the latest radiology advancements impacting medical imaging in 2024?
Recent technological advances are improving diagnostic precision, workflow and patient experience. Notable developments include AI‑assisted image analysis, photon‑counting CT and expanded teleradiology and cloud PACS solutions. AI helps prioritise urgent studies, automate measurements and flag potential abnormalities to speed reporting, while photon‑counting detectors improve spatial resolution and contrast‑to‑noise at lower radiation doses. Telemedicine and cloud image sharing expand access to specialist reads and speed multidisciplinary collaboration across regional networks. These trends offer faster diagnosis, fewer repeat studies and more consistent report quality—clinicians should discuss with imaging providers how new technologies influence turnaround and diagnostic pathways.
How is AI improving diagnostic accuracy and efficiency in radiology?
AI can boost efficiency by automating routine measurements, pre‑populating structured reporting elements and triaging studies with potential urgent findings to the top of the radiologist’s worklist—reducing turnaround times and freeing radiologists to focus on complex cases. Validated AI tools can detect nodules, haemorrhage or fractures with high sensitivity in specific use cases, but they require clinical validation, ongoing monitoring and radiologist oversight to limit false positives and preserve accountability. When integrated responsibly, AI is an assistive tool that augments radiologist interpretation rather than replacing it; responsible deployment includes diverse training datasets, regulatory compliance and periodic performance audits. AI delivers best results when combined with quality image acquisition and a clear clinical question.
What new imaging technologies are available at Life Medical Imaging Central Coast?
Life Medical Imaging Central Coast has invested in advanced capabilities described across our service summaries—most notably ultra‑low dose CT and dedicated women’s and cardiac imaging pathways that broaden diagnostic options for Central Coast patients. Ultra‑low dose CT provides a lower radiation alternative for suitable indications, while cardiac CT angiography supports non‑invasive coronary assessment when clinically justified. Our use of modern equipment and NATA accreditation reflects structured quality systems supporting these services. Referrers are encouraged to specify the clinical question on referrals so our teams can select optimised protocols. Patients and referrers should ask about available modalities when booking to ensure the test matches the clinical need.
How does Life Medical Imaging Central Coast support referring doctors and allied health providers?
Strong collaboration between imaging providers and referrers depends on clear referral pathways, timely reporting and availability of interventional procedures that support diagnosis and treatment. We provide image‑guided interventional services—spinal and joint injections, biopsies and aspirations, and platelet‑rich plasma (PRP) therapy—to assist diagnostic clarification and pain management. Rapid report turnaround, structured reports and open communication channels help allied health and specialists apply imaging findings within patient‑centred care plans. Key ways we support referrers and allied health teams are listed below.
- Image‑guided interventional procedures for diagnostic and therapeutic use.
- Structured reporting and timely communication for urgent and routine findings.
- Collaborative protocol selection to support multidisciplinary care.
Below is a summary of common interventional procedures and typical indications to help referrers decide when to refer for image‑guided therapy.
This table clarifies typical indications and reporting expectations for interventional services. The final subsection explains referral logistics and how referrers can access reports.
What interventional procedures are offered for pain management and diagnosis?
Image‑guided spinal injections deliver steroid or local anaesthetic to epidural or facet regions to reduce radicular or axial pain and can help localise pain generators diagnostically. Joint injections under ultrasound or CT guidance place medication precisely inside the joint to treat inflammatory and degenerative conditions while improving diagnostic certainty. Biopsies and aspirations obtain tissue or fluid samples under imaging guidance to increase diagnostic yield and safety compared with blind approaches. PRP injections offer a regenerative option for selected tendinopathies and soft tissue injuries. Referrers should include relevant clinical history and the specific imaging question on referral forms so procedure planning aligns with the intended diagnostic or therapeutic goal.
Selecting the optimal medical imaging modality for therapeutic applications and clinical practice
ABSTRACT: Naeem, Zarah; Bennion, Colette. Imaging & Therapy Practice; Canterbury (May 2016): 5‑9.
Choosing the best modality, 2016
Clear referral information and appropriate clinical indication improve procedure safety and outcomes. The next practical section describes how providers can submit referrals and obtain reports.
How can healthcare providers refer patients and access imaging reports?
Referring clinicians should submit standardised referrals that include clinical history and the specific imaging question to ensure correct protocol selection; urgent referrals must indicate clinical priority so imaging teams can triage appropriately. Reports are returned to the referrer using the imaging provider’s standard clinical communication channels, with urgent critical results phoned through immediately to the requesting clinician. Many imaging centres support electronic image access and clinician retrieval of archived studies for multidisciplinary review. Referrers can request specific report formats or expedited turnaround when clinically necessary. For detailed referral procedures and templates, referrers can contact Life Medical Imaging Central Coast via our published contact options to discuss referral pathways and access arrangements.
Frequently asked questions
What should I expect during my imaging appointment?
Expect a different experience depending on the modality. For CT you lie on a motorised table that moves through the scanner and you may need to hold your breath briefly. MRI is longer and noisier—remaining still inside the scanner is important and ear protection is provided. Ultrasound involves close contact with a transducer and gel, and allows real‑time interaction with the operator. If you have concerns about comfort or claustrophobia, tell staff beforehand so we can arrange appropriate measures.
How can I access my imaging results?
Radiologists send reports to the referring clinician within agreed turnaround times. Urgent results are communicated immediately to the referrer to ensure prompt care. Patients can request copies of reports and images directly from the imaging provider. Knowing the structure of a radiology report—history, technique, findings and impression—helps you focus on the main clinical points when discussing results with your healthcare provider.
Are there any risks associated with medical imaging procedures?
Each modality has specific risks. CT and X‑ray involve ionising radiation, so dose optimisation is applied. MRI does not use radiation but requires screening for metal implants and considered use of contrast. Ultrasound is generally safe, particularly in pregnancy and paediatrics, because it uses sound waves rather than radiation. Discuss any concerns with your referrer or imaging team so they can explain the safety measures in place.
What are the benefits of using low‑dose CT scans?
Low‑dose CT scans reduce radiation exposure while maintaining diagnostic quality—important for patients who may need multiple scans over time, such as in surveillance programs. Techniques like automated exposure control and iterative reconstruction help achieve this balance, enhancing patient safety without compromising diagnostic performance.
How does ultrasound compare to other imaging modalities?
Ultrasound uses high‑frequency sound waves to create real‑time images without ionising radiation, making it ideal for obstetric monitoring and paediatric assessments. Unlike CT and MRI, which provide detailed static cross‑sectional images, ultrasound is particularly useful for dynamic assessments (for example blood flow or tendon movement) and for guiding procedures at point of care. Its portability and immediacy make it valuable in emergency and outpatient settings.
What advancements in medical imaging should patients be aware of?
Recent advances include AI‑assisted analysis that improves efficiency and consistency, and photon‑counting CT that enhances image quality at lower radiation doses. These technologies are helping clinicians reach diagnoses faster and more accurately. Ask your imaging centre which technologies they use and how these might affect your care pathway.
How can I prepare for my imaging appointment?
Preparation depends on the test. For CT with contrast you may need to fast for a few hours. MRI patients should remove metal objects and may need to fast if sedation is planned. Ultrasound often requires a full bladder for pelvic scans or fasting for certain abdominal studies. Follow the specific instructions provided by your referrer or the imaging provider to ensure the best possible results.
Conclusion
Life Medical Imaging Central Coast offers a wide range of advanced imaging services designed to improve diagnostic accuracy and patient care. By understanding the strengths of each modality, patients and clinicians can make informed choices tailored to individual needs. If you’re unsure which test is right, contact our team for personalised guidance—we’re here to help you choose the most appropriate imaging option and to support safe, timely care on the Central Coast.