Pain Management Injections: Types, Benefits, and Procedures for Effective Pain Relief
Pain management injections are minimally invasive procedures that deliver medication or biologic therapies directly to the site of musculoskeletal or spinal pain. They can reduce inflammation, interrupt pain signals and — in some cases — support tissue healing. This page explains the most common injection options — including epidural steroid injections, facet joint injections, nerve blocks, corticosteroid and hyaluronic acid injections, and platelet‑rich plasma (PRP) therapy — when each is used, and what you can expect before, during and after treatment. You’ll learn how each approach works, the relative advantages, typical timelines for relief, and why imaging guidance (ultrasound or X‑ray/fluoroscopy) improves accuracy and safety. We also cover benefits and risks, step‑by‑step preparation and recovery tips, and how image‑guided delivery fits into a broader care plan with physiotherapy and specialist referral. Practical checklists and clear comparison tables are included to help patients and referrers make informed choices about injection treatment.
What Are the Different Types of Pain Management Injections?
Pain management injections include several targeted procedures used either to help diagnose the pain source or to provide therapeutic relief. Many combine a local anaesthetic for immediate numbness with an anti‑inflammatory such as a corticosteroid, while others use regenerative or lubricating agents like PRP or hyaluronic acid for longer‑term benefit. Imaging guidance — ultrasound for soft tissues and X‑ray/fluoroscopy for spinal targets — helps ensure accurate needle placement, reduces complications and improves outcomes. The list below summarises the most commonly offered injection types for back pain, joint osteoarthritis and soft tissue injuries.
Common injection categories include:
- Epidural steroid injections: Reduce inflammation around spinal nerve roots to relieve sciatica and radicular pain.
- Facet joint injections: Deliver medication into the small joints at the back of the spine to diagnose or treat facet arthropathy and axial back pain.
- Nerve block injections: Temporarily interrupt pain signals for neuropathic or regional pain conditions.
- Joint injections (corticosteroid / hyaluronic acid / PRP): Treat osteoarthritis and tendinopathy using anti‑inflammatory, lubricating or regenerative approaches.
- Trigger point injections and soft‑tissue injections: Target local muscle or tendon pain using local anaesthetic with or without anti‑inflammatory agents.
To compare typical uses and expected duration of relief across these options, the table below summarises key features.
This comparison shows how the right injection depends on the target tissue, the underlying problem and whether the goal is fast anti‑inflammatory relief or longer‑term regenerative benefit. The next section reviews how epidural steroid injections work for back and neck pain.
How Do Epidural Steroid Injections Relieve Back and Neck Pain?
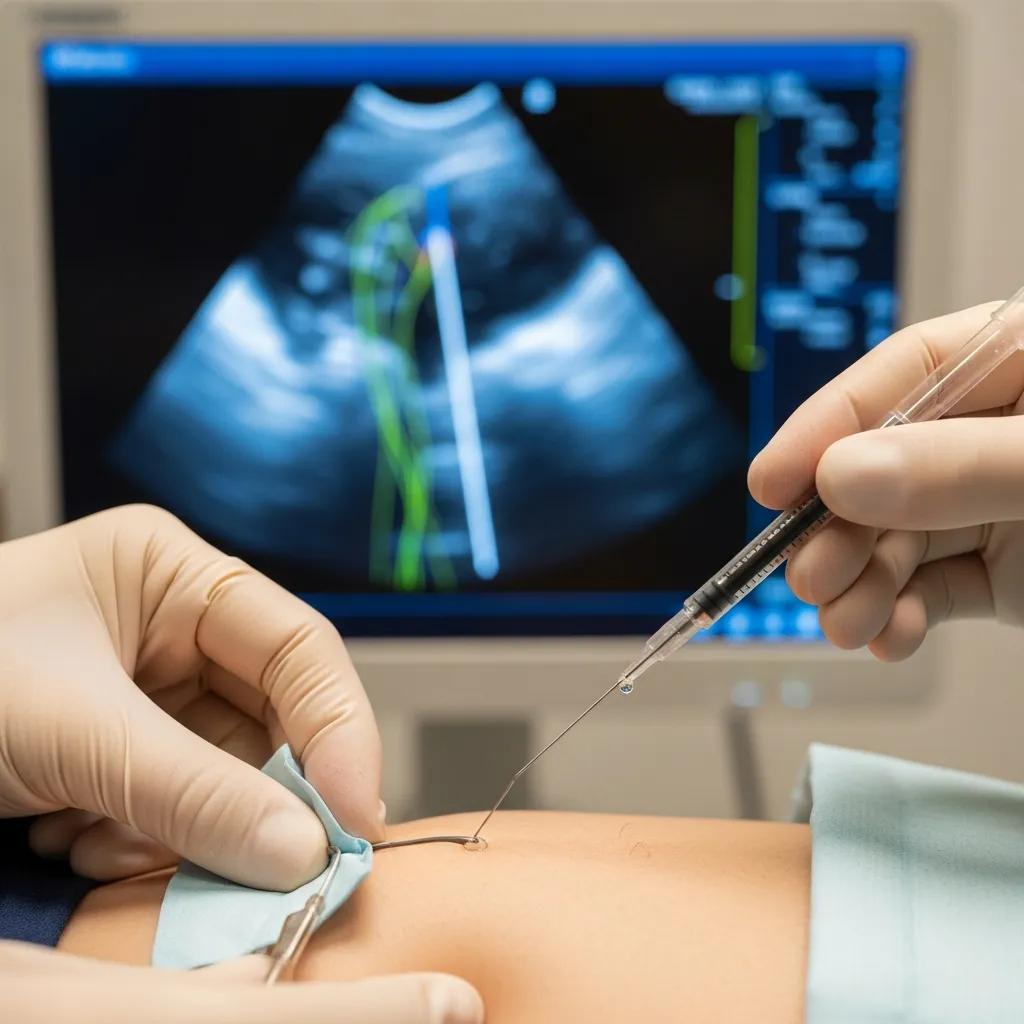
Epidural steroid injections place a corticosteroid — often combined with a local anaesthetic — into the epidural space around spinal nerve roots to reduce perineural inflammation and nerve irritation. The steroid decreases inflammatory mediators that sensitize nerve tissue, while the anaesthetic gives rapid, temporary pain relief useful for diagnosis and early mobilisation. Performed under fluoroscopic (X‑ray) guidance, the needle is positioned precisely in the epidural space to maximise benefit and minimise risk. Many patients notice pain reduction within 24–72 hours, with full effect sometimes developing over one to two weeks. Results range from brief relief to sustained improvement over months; repeat injections or further interventions such as physiotherapy or specialist referral are considered based on response.
Epidural injections can also be diagnostic: if pain improves after the injection, it helps confirm the affected nerve root and guides next steps — which may include surgical review or radiofrequency procedures if relief is temporary.
What Are Facet Joint Injections and Their Role in Spinal Pain Relief?
Facet joint injections target the small synovial joints at the back of the spine that can become painful with degenerative change. A facet injection may be diagnostic — using local anaesthetic to see if the joint is the pain source — or therapeutic when a corticosteroid is added to reduce inflammation. Ultrasound or X‑ray guidance helps the clinician place the needle into the joint or adjacent space accurately, improving diagnostic clarity and treatment precision while reducing the chance of misplaced injections. When a diagnostic block gives clear short‑term relief, a referral for radiofrequency denervation may follow to provide longer‑lasting symptom control.
Facet injections are especially useful for patients with focal posterior spinal pain. They help identify the pain source and provide short‑term symptom control so patients can take part in rehabilitation.
How Do PRP Therapy and Joint Injections Help Manage Musculoskeletal Pain?
PRP therapy and joint injections work by different mechanisms: corticosteroids act quickly to reduce inflammation; hyaluronic acid improves joint lubrication and mechanics; and PRP delivers concentrated growth factors from the patient’s own blood to encourage tissue repair. PRP is prepared by drawing blood, concentrating platelets with a centrifuge, then injecting that concentrate into the injured tendon or arthritic joint under imaging guidance to ensure accurate placement. Hyaluronic acid (viscosupplementation) aims to improve joint biomechanics in osteoarthritis, while steroids suppress inflammatory pathways to reduce pain and swelling. The choice between these options depends on the condition (for example, tendinopathy versus advanced osteoarthritis), patient goals and prior treatment response.
To make expected timelines and typical indications clear, the table below summarises mechanism, indications and onset for PRP and common joint injections.
This comparison highlights that PRP is regenerative and slower to act but may change tissue biology, whereas steroids provide faster anti‑inflammatory relief and hyaluronic acid targets joint mechanics. The next section outlines how PRP is prepared and what evidence shows about expected outcomes.
What Is Platelet-Rich Plasma Therapy and How Does It Promote Healing?
Platelet‑rich plasma (PRP) concentrates a patient’s own platelets to deliver higher levels of growth factors and signalling proteins into injured tendons, ligaments or early osteoarthritic joints. We draw a sample of blood, centrifuge it to concentrate platelets, then inject the PRP under ultrasound guidance so the treatment reaches the affected tissue accurately. Up to 2024, research suggests PRP can improve tendon healing and reduce pain in selected conditions compared with placebo or steroids, although study methods and results vary. PRP is generally well tolerated because it is autologous, but patients should expect gradual improvement over several weeks and, in some cases, a course of more than one injection.
Knowing how PRP works helps clinicians and patients set realistic expectations and combine the therapy with rehabilitation for the best functional outcome.
Which Joint Injections Are Used for Arthritis and Tendinopathy?
For arthritis and tendinopathy the main injection options are corticosteroids (for rapid anti‑inflammatory effect), hyaluronic acid (for joint lubrication) and PRP (for regenerative stimulation). Corticosteroids are commonly used for acute flares and give faster symptom relief but may have reduced benefit with frequent repeats. Hyaluronic acid is often used for knee osteoarthritis and can provide months of symptom relief in some patients. PRP is preferred for many tendon disorders and early osteoarthritis where tissue modulation is the goal; it typically produces slower, progressive improvement and is most effective when combined with a structured physiotherapy program.
Clinicians choose the best option by considering joint severity, prior treatment response, activity goals and the role of imaging guidance to ensure accurate, safe delivery. The next section explains nerve block injections and their specific uses.
How Do Nerve Block Injections Provide Targeted Pain Relief?
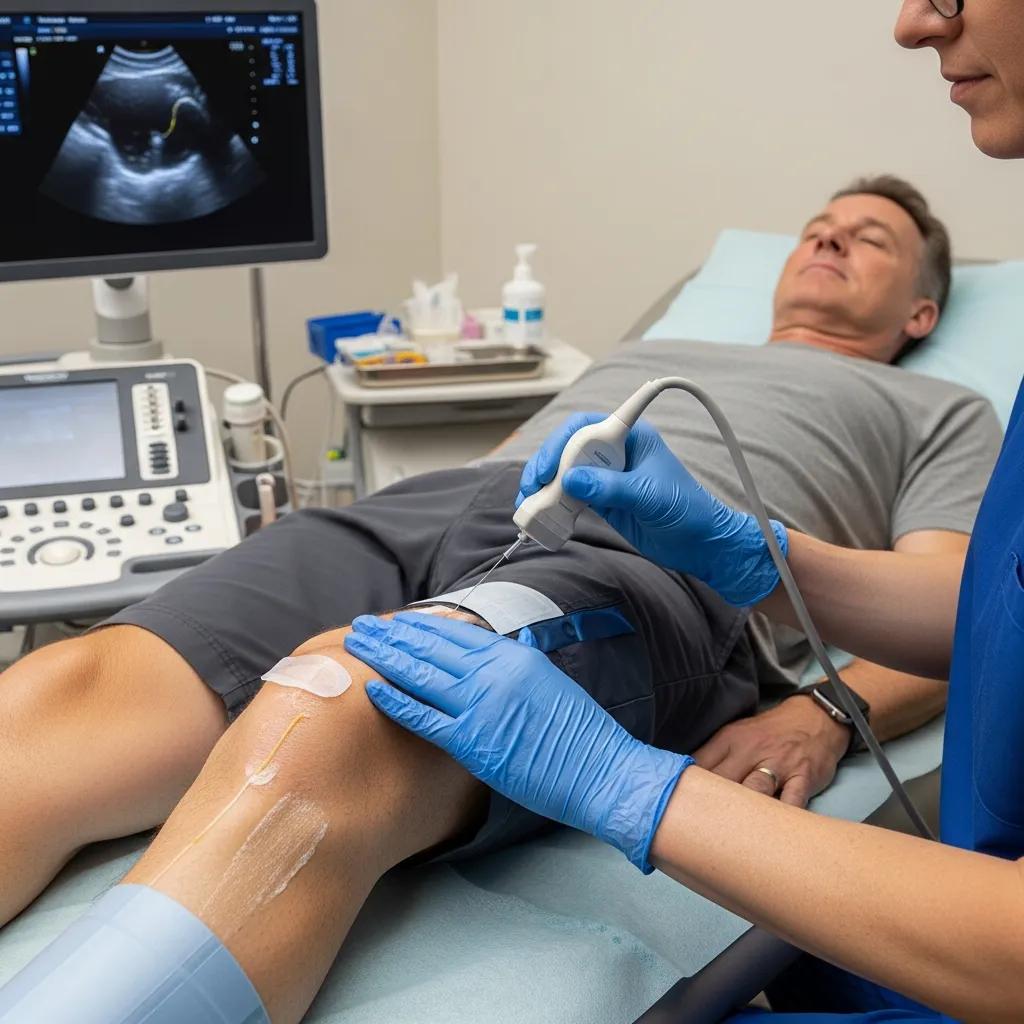
Nerve block injections temporarily stop pain signals by delivering a local anaesthetic — sometimes combined with a steroid — around specific peripheral nerves or plexuses. They are used both diagnostically and therapeutically for neuropathic and regional pain syndromes. Blocks can help localise the pain source, guide surgical planning or provide medium‑term relief that enables rehabilitation and physiotherapy. Imaging guidance — ultrasound for peripheral nerves and X‑ray/fluoroscopy for deeper neural targets — supports precise injection, minimises tissue trauma and reduces the risk of vascular or neural injury. Below are common conditions treated with nerve blocks and what to expect from the procedure.
Common conditions treated by nerve blocks include:
- Peripheral neuropathic pain and nerve entrapment syndromes.
- Complex regional pain syndrome and chronic regional pain.
- Diagnostic blocks prior to surgical planning or neuroablation.
These indications place nerve blocks within a larger care pathway where diagnostic clarity and symptom control guide next steps; the following section describes specific conditions in more clinical detail.
What Conditions Can Nerve Block Injections Treat?
Nerve blocks can help with a variety of painful conditions, including neuropathic pain from nerve entrapment, acute postoperative neuralgia, complex regional pain syndrome, and as diagnostic tests when a nerve origin is suspected. For example, a selective nerve or plexus block can confirm whether a peripheral nerve is the primary pain source and whether neuroablation or surgery might be appropriate. Patient responses vary: some experience immediate, strong analgesia from local anaesthetic alone, while others get longer relief when a steroid is added. A successful block often leads to multidisciplinary follow‑up such as physiotherapy, pain specialist review or targeted interventions once pain allows rehabilitation.
A clear diagnostic response to a nerve block helps clinicians plan definitive treatment and decide on repeat procedures or referrals.
What Is the Procedure for Ultrasound and X-ray Guided Nerve Block Injections?
The guided nerve block procedure starts with informed consent, infection screening and positioning to expose the target area. Real‑time ultrasound or X‑ray imaging is used to identify landmarks and plan the needle path. Under sterile conditions, the operator advances a fine needle to the perineural space with live imaging, injects local anaesthetic with or without steroid while observing spread, and monitors the patient for immediate effect and any adverse reaction. After the procedure patients are usually observed for 20–30 minutes before discharge and receive written aftercare instructions, including pain management and activity advice. Imaging guidance reduces needle passes, improves accuracy compared with blind techniques, lowers complication risk and supports better clinical outcomes.
This stepwise explanation helps patients know what to expect on the day and why imaging‑guided delivery is recommended.
What Are the Benefits and Risks of Pain Management Injections?
Pain management injections can provide targeted relief from pain and inflammation, improve mobility and function, and often enable a rehabilitative programme that addresses the causes of pain. They are typically part of a broader care plan alongside physiotherapy, activity modification and specialist assessment rather than standalone cures. Injections do carry risks — common minor effects include a transient pain flare at the injection site, while rare but serious complications include infection or neurological injury — so risk reduction through sterile technique, appropriate dosing and imaging guidance is essential. The table below summarises benefits, common side effects and mitigation strategies to help weigh the trade‑offs.
This structured overview shows that while benefits can be significant, careful patient selection and strict procedural standards reduce risk. The next section explains how injections translate into improved mobility and less inflammation.
How Do Pain Injections Improve Mobility and Reduce Inflammation?
Injections improve mobility mainly by reducing the pain and inflammation that limit movement, allowing patients to participate more fully in physiotherapy and functional rehabilitation. Corticosteroids reduce cytokine‑mediated inflammation and perineural swelling, often producing rapid pain relief and improved range of motion. PRP’s growth factors may alter the local biological environment to support tendon repair and better load tolerance over weeks to months, helping longer‑term recovery. By interrupting the pain–disuse cycle, injections enable progressive loading, strengthening and retraining that address the mechanical contributors to disability.
Restored mobility after injections commonly leads to increased activity and reduced reliance on analgesics, but lasting benefit depends on integrating injections with rehabilitation.
What Are the Potential Side Effects and How Can They Be Minimized?
Common side effects include temporary soreness at the injection site, minor bruising, a short‑lived increase in pain (post‑injection flare) and transient systemic effects from corticosteroids (for example mood or blood‑sugar changes in susceptible people). Rare but serious complications include infection, bleeding and nerve injury. These risks are reduced by strict sterile technique, pre‑procedure screening (including review of anticoagulant medications when relevant), use of imaging guidance and sensible dosing intervals. Patients should be told about red flags — fever, worsening neurological symptoms or uncontrolled pain — and advised to seek urgent medical review if they occur. Routine follow‑up helps identify and manage any adverse effects early.
Clear pre‑procedure counselling and risk‑reduction practices are central to safe, confidence‑building care.
How Should Patients Prepare for Pain Management Injections and What to Expect Afterwards?
Preparation commonly includes a medication review (notably anticoagulants), screening for active infection and confirmation of referral and consent. Instructions vary by injection type: PRP requires a blood draw on the day of the procedure, while many spinal injections require only local anaesthesia with no fasting. If sedation is planned you may be asked to fast and arrange transport. On the day expect arrival, consent review, imaging‑guided needle placement and a short monitoring period — most people go home the same day with simple aftercare instructions. Post‑procedure care usually involves rest for 24–48 hours, a gradual return to activity guided by symptoms, and timely physiotherapy to maximise recovery.
Practical checklists below outline common pre‑procedure steps and realistic recovery timelines to help you plan.
Pre‑procedure checklist:
- Bring your referral and any completed consent forms.
- Tell us all medications you take, especially anticoagulants or immunosuppressants.
- Follow any fasting or sedation instructions provided by the clinic.
- Arrange transport if sedation or significant immediate analgesia is expected.
Aftercare timeline and expectations:
- First 24–72 hours: you may have soreness or a short‑lived flare; use ice and simple analgesics as advised.
- 1–2 weeks: many patients notice early improvement after corticosteroid injections; PRP benefits may start to emerge.
- 2–6 weeks: progressive functional gains and commencement or escalation of physiotherapy as pain allows.
These steps help set realistic expectations for recovery and follow‑up. If you are on the Central Coast and seeking image‑guided injection services, Life Medical Imaging Central Coast offers spinal and joint injections, PRP therapy and image‑guided biopsies — bookings and referrals can be arranged through the clinic’s phone or email.
What Are the Pre-Procedure Guidelines for Different Injection Types?
Guidelines vary by injection but typically include a medication review (especially anticoagulants), screening for active infection, and confirmation of referral and consent. For PRP, a blood draw is performed just before the procedure, so it helps to be well hydrated and follow any clinic‑specific instructions; general anaesthesia is not required. Spinal procedures may require review of recent imaging and clear identification of the target level; some clinics give fasting instructions if sedation is planned. Clear communication between the referrer, patient and imaging team ensures safe scheduling and appropriate preparation.
Following these guidelines reduces procedural risk and helps create optimal conditions for accurate, image‑guided therapy.
What Is the Recovery Process and Post-Injection Care?
Recovery usually begins with a short observation period, followed by home rest and symptom‑guided activity modification. Most patients resume normal activities within a few days but should avoid heavy lifting for a short period. Use simple analgesics or anti‑inflammatories as directed for transient discomfort. Physiotherapy is commonly recommended once pain allows, to consolidate mobility gains. Expect a possible transient pain flare for 24–72 hours and understand when to seek urgent care for fever, worsening neurological signs or uncontrolled pain. Follow‑up appointments assess response and guide repeat treatments or onward referral if needed.
A clearly defined recovery plan helps you move safely from the procedure into rehabilitation and longer‑term management.
Why Choose Life Medical Imaging Central Coast for Pain Management Injections?
Life Medical Imaging Central Coast is a NATA‑accredited, independent radiology clinic on the Central Coast, NSW. We offer a focused interventional and pain management service that combines image‑guided precision with streamlined referral pathways. Our team performs spinal and joint injections, PRP therapy, biopsies and aspirations using ultrasound and X‑ray guidance to improve accuracy and safety. Procedures are delivered by experienced radiologists trained in interventional techniques. NATA accreditation reflects recognised standards for imaging, specimen handling and quality systems, supporting consistent procedural governance. For patients and referrers on the Central Coast, we accept referrals and can arrange appointments — please contact the clinic by phone or email for bookings and enquiries.
How Does Advanced Imaging Technology Enhance Injection Accuracy?
Real‑time ultrasound for soft‑tissue and peripheral nerve targets, and fluoroscopy/X‑ray for spinal procedures, allow direct visualisation of anatomy, needle trajectory and injectate spread — greatly improving targeting accuracy versus blind techniques. Ultrasound shows nerves, tendons and nearby vessels so the operator can avoid inadvertent injury and place treatment precisely. Fluoroscopy confirms needle position and contrast spread for epidural and selective nerve‑root procedures. These modalities often reduce needle passes, speed the procedure and contribute to better clinical outcomes through precise delivery.
Overall, imaging guidance makes injections safer, more reproducible and more effective for both diagnosis and therapy.
What Expertise and Accreditation Support Quality Care at Life Medical Imaging?
Our team at Life Medical Imaging Central Coast includes radiologists and imaging staff experienced in interventional procedures, working within a NATA‑accredited framework that underpins quality assurance and standard operating procedures. Accreditation and clinical governance ensure imaging, specimen handling (where relevant) and equipment calibration meet external standards, supporting patient safety and consistent procedural quality. We emphasise collaboration with referring GPs and specialists so referrals, imaging and interventions are coordinated with a patient’s broader care plan. For local patients on the Central Coast seeking image‑guided pain management, the clinic provides a clear pathway for bookings and referrals via the publicly listed phone and email.
This combination of technical skill, accreditation and local access allows us to deliver image‑guided injection services as part of an integrated patient‑care pathway.
Frequently Asked Questions
What should I expect during a pain management injection procedure?
When you come for an injection we’ll review your medical history and confirm informed consent. The procedure is performed using imaging (ultrasound or X‑ray) to position the needle accurately. A local anaesthetic is usually given to reduce discomfort, followed by the therapeutic injection. After the procedure you’ll be observed briefly and given written aftercare instructions to support recovery.
How long does it take to see results from pain management injections?
Timing varies by injection type and by patient. Corticosteroid injections often provide relief within a few days, with peak effect typically in 1–2 weeks. Regenerative treatments like PRP are slower, with gradual improvement expected over 4–12 weeks. Discuss your expected timeline with your clinician so you have realistic goals for recovery.
Are pain management injections suitable for everyone?
Not everyone is a candidate. Factors such as the type of pain, underlying health conditions and previous treatment responses determine suitability. Active infection, bleeding disorders or allergies to injection components can exclude patients from some procedures. A thorough assessment by a clinician will determine whether injections are appropriate as part of a personalised care plan.
What are the costs associated with pain management injections?
Costs vary depending on the type of injection, the facility and whether imaging guidance is used. Insurance or Medicare arrangements may affect out‑of‑pocket costs. We recommend checking with your insurer about coverage and contacting the clinic for a specific fee estimate before booking.
How can I prepare for a pain management injection?
Preparation usually includes a medication review, especially anticoagulants, and disclosure of allergies and medical history. Follow any fasting instructions if sedation is planned and arrange transport if needed. Arriving prepared helps ensure a smooth procedure and optimal results.
What follow-up care is needed after a pain management injection?
Follow‑up care is important to monitor recovery and assess treatment effect. You’ll typically be advised to rest for 24–48 hours and return to activities gradually as comfortable. Track any changes in pain or mobility and report them to your clinician. Follow‑up appointments may be arranged to evaluate progress and decide on further treatment if needed.
Conclusion
Pain management injections provide targeted options to reduce pain, improve mobility and support rehabilitation. Whether it’s an epidural steroid injection, PRP therapy or a nerve block, treatments can be tailored to your needs and goals. Understanding the benefits, risks and preparation helps you make informed choices about your care. For expert advice and to explore our image‑guided injection services, contact Life Medical Imaging Central Coast to arrange a consultation or referral.

