UK Healthcare System: How Patient Pathways and Diagnostic Imaging Work
The UK’s healthcare network combines a national, publicly funded system with private options that together determine how people access imaging tests like CT, MRI, ultrasound and X‑ray. This guide breaks down how services are organised, how patients move through NHS pathways, who decides on scans and how requests are prioritised. Knowing these steps matters: timely imaging speeds diagnosis and treatment planning, and understanding the choices available helps patients and referrers make smarter decisions. You’ll find clear explanations of national and regional structures, a step‑by‑step NHS pathway, practical notes on common imaging tests and preparation, routes to private imaging, and how funding and insurance affect access. Practical checklists and summaries of safety and ethical standards are included to help patients and clinicians navigate diagnostic imaging with confidence.
What Is the Structure of the UK Healthcare System?
The UK healthcare system is built around the National Health Service (NHS), a publicly funded framework that organises care at national, regional and local levels. Policy and regulation are set nationally, while regional bodies and Integrated Care Systems (ICSs) plan local services, workforce and diagnostic capacity. This tiered approach affects where imaging is available, how resources are distributed and how patients move between primary care, community services and hospitals. Understanding these layers explains why scan availability and wait times can differ by area, and why collaboration between providers can sometimes speed access. The sections below outline how primary and secondary care fit together and how ICSs shape diagnostic pathways.
How Does the National Health Service Organise Care Delivery?
Primary care — usually led by GPs — is the main gateway for most imaging requests. When a clinician decides a scan is needed they send a referral, typically via electronic systems, that includes clinical history and urgency. Hospitals and diagnostic centres carry out the scans and produce reports. Services are coordinated so community clinics, outpatients and acute hospitals can share imaging capacity where possible. Recent reforms focus on joined‑up referrals to cut duplication and speed reporting. Ultimately, the referral‑to‑report flow depends on available staff and equipment, which are shaped by regional planning and commissioning choices.
Improving General Practitioner Access to Diagnostic Imaging in the UK
Direct access to diagnostic imaging from General Practice can reduce referrals to hospital specialists and emergency departments and speed diagnosis. Enhanced GP access to imaging has the potential to lower hospital admissions, improve patient care and support better outcomes. This scoping review summarises evidence on the value and impact of direct GP access to radiological services.
Impact of enhancing GP access to diagnostic imaging: a scoping review, A Phelan, 2023
What Are Integrated Care Systems and Their Impact on Patient Services?
Integrated Care Systems (ICSs) bring local health and care organisations together to plan services around population needs. By aligning budgets, workforce planning and care pathways, ICSs can reduce fragmentation and improve access to diagnostics. Practical measures include pooled resources for diagnostic hubs, shared imaging rotas and standardised referral protocols. For patients this can mean clearer referral routes, faster triage and better transparency about where and when scans will take place — though how quickly these changes appear varies by area and depends on cooperation between GPs, hospitals and independent providers.
How Do NHS Patient Pathways Work for Diagnostic Imaging?
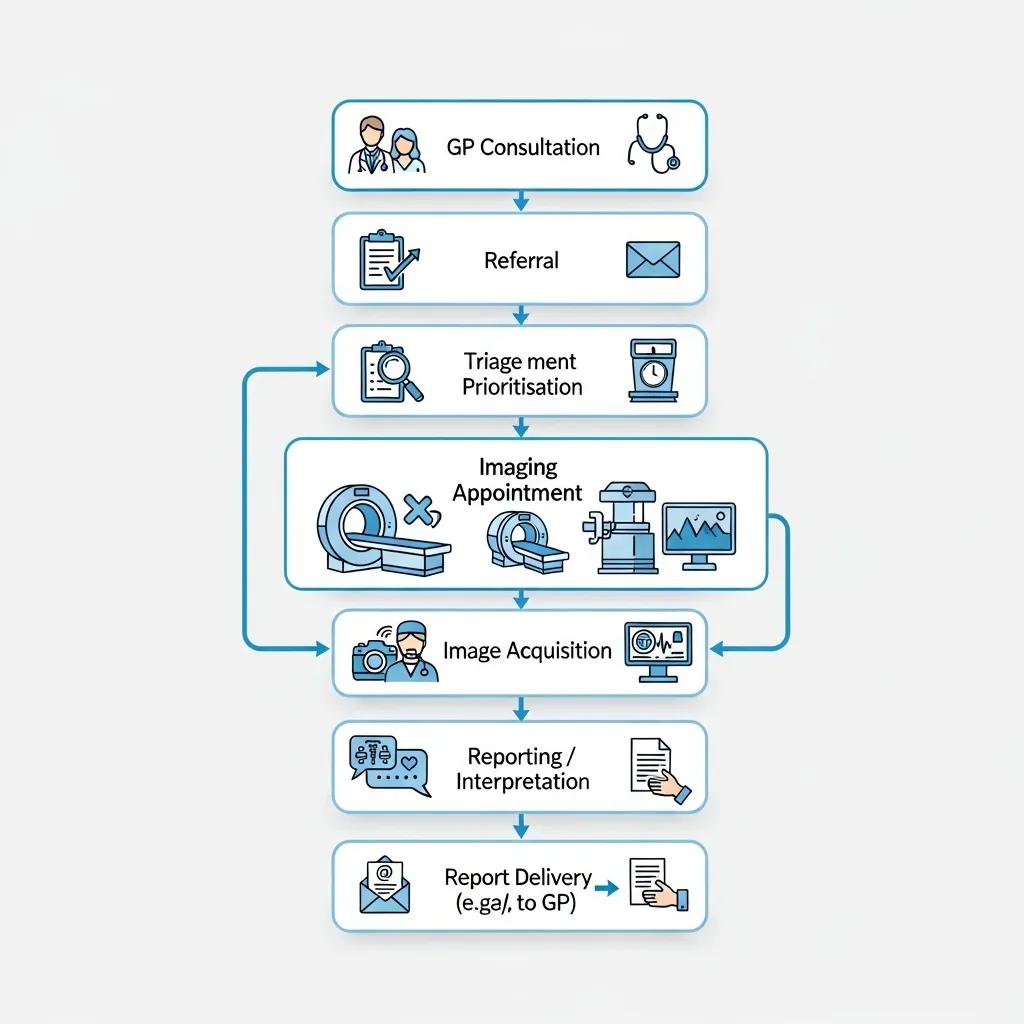
In the NHS, diagnostic imaging follows a predictable sequence: presentation, referral, triage, booking, scanning and report delivery. Each step involves different professionals and expected timeframes so urgent cases are handled quickly. Referrers apply clinical justification when ordering a scan, radiology teams triage requests by urgency and suitability, and patients receive appointment and preparation details from the provider. Results are sent back to the referring clinician, with urgent findings escalated directly. Below is a concise, step‑by‑step pathway you can use as a quick reference.
- Presentation and Initial Assessment: The patient sees a GP or clinician who assesses symptoms and decides whether imaging will help confirm a diagnosis or guide treatment.
- Referral Submission: The clinician completes an electronic or paper referral that outlines the clinical history and urgency; referrals can come from GPs, A&E or specialists.
- Triage and Prioritisation: Radiology staff review referrals, assign urgency categories and schedule scans so urgent requests are fast‑tracked.
- Booking and Preparation: The imaging provider contacts the patient with the appointment time and any preparation instructions (for example fasting or removing metal objects).
- Scan and Reporting: A radiographer or sonographer carries out the scan. A radiologist interprets the images and issues a formal report to the referring clinician.
- Results and Follow‑up: The referring clinician reviews the report, explains findings to the patient and arranges treatment or further tests if needed.
This numbered pathway explains who does what at each stage and what patients should expect, including how to get help if symptoms change or worsen.
What Are the Steps for Accessing Medical Imaging Through the NHS?
Access starts with a clinical assessment: a GP or hospital clinician decides if imaging is justified and submits a referral with the suspected diagnosis and relevant history. Radiology teams triage referrals and assign appointment slots based on urgency. Patients receive clear instructions on preparation and arrival. At the appointment, trained staff collect any needed clinical details and perform the study under safety protocols. A radiologist then prepares a formal report and sends it to the referring clinician, who discusses results and next steps with the patient. Knowing this sequence helps set expectations for timing and follow‑up.
How Are Urgent and Routine Imaging Requests Managed in the UK?
Requests are prioritised through clinical triage systems using set criteria that reflect likely clinical impact. Urgent categories cover potentially life‑ or limb‑threatening conditions; routine categories are for diagnostic clarification or monitoring. Radiology departments use escalation protocols so urgent cases can be inserted into early lists or moved across a network with available capacity. Good communication between referrers and radiology teams is essential to ensure correct prioritisation. If a patient’s symptoms change, clinicians can request re‑triage to speed up assessment.
What Are the Common Types of Diagnostic Imaging Services Available in the UK?
Common imaging modalities include CT, MRI, ultrasound and X‑ray. Each works differently, suits different clinical questions and has its own preparation needs. CT (computed tomography) uses X‑rays and computer reconstruction for detailed cross‑sectional images, useful in trauma and abdominal or chest assessment. MRI (magnetic resonance imaging) uses magnetic fields for excellent soft‑tissue detail, often chosen for brain, spine and joint problems. Ultrasound uses sound waves for real‑time imaging of soft tissues, vessels and pregnancy with no ionising radiation. Digital X‑ray is fast and effective for bone and chest imaging. The table below summarises typical uses and preparation points to help patients and clinicians choose the right test.
Different modalities suit different clinical problems and come with specific preparation and safety notes.
This comparison shows why the choice of modality depends on the clinical question, patient factors and how quickly results are needed.
What Are the Four Main Types of Medical Imaging?
The four main types — CT, MRI, ultrasound and X‑ray — cover most diagnostic needs and differ in how images are made, their clinical uses and safety profiles. CT is fast and detailed for acute and vascular problems. MRI gives superior soft‑tissue contrast without ionising radiation but takes longer. Ultrasound is portable and safe in pregnancy, offering live assessment of organs and blood flow. Digital X‑ray is quick and widely available for bones and chest imaging. Knowing these differences helps referrers select the most appropriate test and helps patients understand why one scan is chosen over another.
How Do Radiologists Support Diagnosis Through Imaging?
Radiologists interpret images, combine findings with clinical information and produce reports that guide treatment and follow‑up. Sub‑specialist radiologists add focused expertise for areas such as paediatrics, cardiac or musculoskeletal imaging. Typically, radiographers acquire the images and radiologists review them, compare with prior studies, list likely diagnoses and recommend next steps (for example further imaging or biopsy). Radiologists also take part in multidisciplinary meetings and advise on image‑guided procedures. Clear communication between radiologists and referrers ensures images translate into timely clinical decisions.
How Can Patients Access Private Medical Imaging Services in the UK?
Private imaging is available through clinician referral, insurer authorisation or self‑referral to independent centres. It can be a practical alternative when NHS wait times are long or when patients want specific appointment times or technology. Private providers often offer quicker booking, flexible appointment slots and access to particular scanners or sub‑specialist reporting. If you consider private imaging, check your insurer’s cover, ask for a clear price estimate and confirm how results will be shared with your NHS or private clinician so care remains coordinated.
Private providers can complement NHS services. The list below summarises common benefits patients seek when choosing private imaging.
- Faster access: Appointments are often sooner than routine NHS slots.
- Flexible scheduling: You may be able to pick times that fit your schedule.
- Choice of provider or technology: Access to specific scanners or sub‑specialist reporting can be available.
These benefits make private imaging a useful option for those prioritising speed or choice, while keeping in mind cost and continuity of care.
What Are the Benefits of Choosing Private Diagnostic Imaging?
Private imaging can reduce waiting times, offer more appointment flexibility and sometimes provide access to advanced or low‑dose equipment for high‑quality images. Faster scans may lead to quicker decisions and earlier treatment, which can be important if NHS capacity is limited or if a second opinion is needed. Private reports can be shared with the referring NHS clinician to keep care integrated. Before booking, confirm costs and insurer coverage so you understand the trade‑offs between speed, price and continuity with your usual care team.
How Does Private Imaging Complement NHS Services?
Private imaging adds capacity, specialist second opinions and scheduling options while still allowing results to be shared with NHS teams. Providers commonly transfer reports and digital images to referrers so private scans can inform NHS treatment plans and help avoid delays. In many cases private imaging speeds up diagnosis and treatment, but whether it’s a practical option depends on funding and insurance arrangements. Understanding how private and NHS services interact helps patients and clinicians choose the best route for individual needs.
What Are Patient Rights and Healthcare Access Considerations in the UK Health System?
Patients in the UK have rights to choice of provider, informed consent, access to their records and a complaints process — all of which apply to diagnostic imaging. Informed consent should cover the reason for the scan, potential risks (for example radiation exposure when relevant) and any preparation required. Patients can request copies of reports and images through their clinician or provider. Accredited services, trained staff and radiation protection measures are standard expectations. The sections below outline how to choose a provider and what safety and ethical standards you should expect.
How Can Patients Choose Their Imaging Provider?
Choosing an imaging provider means looking at accreditation, staff expertise, the technology available, turnaround times and practical details like location and appointment options. Prefer providers with recognised accreditation and clear reporting pathways, ask about low‑dose or advanced imaging choices when relevant, and check expected timelines for results. Confirm how reports will be shared with your referrer to maintain continuity of care. Also consider ease of booking, preparation instructions and support for mobility or child patients when making your choice.
What Are the Ethical and Safety Standards in Medical Imaging?
Safety and ethics in imaging focus on justifying and optimising radiation dose, obtaining informed consent, protecting patient privacy, and ensuring staff training and external quality assurance. Radiology services must justify exposures, apply dose‑reduction techniques where appropriate (for example low‑dose CT protocols), and follow consent procedures for higher‑risk tests. Regular audits and accreditation support ongoing quality improvement. Patients should expect clear explanations of risks and benefits, special protocols for vulnerable groups such as children, and straightforward ways to raise concerns.
How Is Diagnostic Imaging Funded and Reimbursed Within the UK Health System?
Diagnostic imaging funding in the UK is mainly through public NHS budgets, with private insurance and self‑pay options as supplements. NHS funding covers clinically justified imaging but can be limited by budget and workforce availability, which affects wait times and equipment investment. Private insurance may cover scans subject to policy terms and pre‑authorisation, and self‑pay patients can book directly with independent providers. Each payment route affects where and how quickly imaging happens; the table below summarises typical coverage and referral requirements for each payer type.
Different payers influence access, timing and provider choice for imaging services.
Use this comparison to confirm likely timelines and administrative steps before booking a scan.
What Role Does Public Funding Play in NHS Imaging Services?
Public funding determines how many scans the NHS can deliver, where specialised equipment is located and how many staff are available to report studies. Budget limits or competing priorities can slow capital investment in new scanners or expansion of reporting capacity, which affects routine waiting times. Policy initiatives and regional planning, such as diagnostic hubs, aim to increase throughput and reduce variation, but changes take time and depend on local decisions.
How Do Private Insurance and Out-of-Pocket Payments Affect Access?
Private insurance can speed access by authorising and funding scans, while self‑pay patients can arrange immediate imaging with independent providers for a clear fee. Always check policy exclusions, authorisation processes and any excesses or co‑payments. Confirm your chosen provider accepts your insurer and will provide a report suitable for sharing with NHS clinicians. If you self‑pay, ask for transparent billing and electronic copies of images and reports so your care remains coordinated.
- Check your funding route: Confirm NHS referral status, insurer authorisation or self‑pay arrangements before booking.
- Verify report transfer: Ensure the provider will send results to your clinician for ongoing care.
- Ask about turnaround: Get expected timelines for the scan and the formal report so you know what to expect.
These simple steps help privately funded imaging fit smoothly into broader clinical care.
For patients or referrers seeking private options with a broad service menu and up‑to‑date equipment, Life Medical Imaging Central Coast illustrates how an independent radiology clinic can complement NHS services. The clinic offers general CT, cardiac CT, CT angiography, dental imaging, digital X‑ray, a range of ultrasounds (including obstetric and vascular), interventional procedures, paediatric imaging and DEXA bone densitometry. It highlights low‑dose, high‑definition equipment, NATA accreditation and sub‑specialist reporting — examples of how private providers can speed access while maintaining quality and coordinated reporting.
- Confirm clinical justification: Even when paying privately, ensure your clinician documents the indication so results integrate with ongoing care.
- Request clear estimates: Ask providers for transparent pricing and what’s included (images, formal radiologist report, any follow‑up).
- Keep records: Obtain electronic copies of images and reports to share with NHS clinicians or other specialists.
Following these steps preserves continuity of care and ensures privately obtained imaging informs subsequent management.
Frequently Asked Questions
What Should Patients Expect During a Diagnostic Imaging Appointment?
At your appointment you’ll check in, confirm medical history and follow any preparation instructions. A radiographer or sonographer will explain the procedure and answer questions. Scan time varies by test — an MRI typically takes longer than an X‑ray. After the scan you’ll be told when results are likely to be available; formal reports are sent to the referring clinician for discussion and next steps.
How Can Patients Prepare for Different Types of Imaging?
Preparation depends on the test. For CT you may need to fast and discuss contrast allergies. For MRI remove metal objects and tell staff about implants. Ultrasound often requires fasting for abdominal exams, while X‑rays usually need little or no preparation. Always follow the specific instructions given by your imaging centre to ensure accurate results and a smooth visit.
What Are the Risks Associated with Diagnostic Imaging?
Imaging is generally safe but carries some risks. CT and X‑ray use ionising radiation; repeated exposure carries a small long‑term risk and is justified only when clinically necessary. MRI uses strong magnets and can be unsafe for some implants or devices. Ultrasound uses sound waves and has no known radiation risk. Discuss any concerns with your clinician before the test so risks are explained and minimised.
How Do Waiting Times for Imaging Vary Across the UK?
Waiting times depend on local demand, NHS funding and resource availability. Urban areas with more facilities may offer shorter waits, while rural areas can experience longer delays. The urgency of your referral is a key factor: urgent cases are prioritised and seen faster. Ask when your referral is made for an expected timeframe so you know what to expect.
What Should Patients Do If They Experience Delays in Receiving Results?
If your results are delayed, first contact the imaging centre where the scan was done to check the status. Confirm whether the report has been sent to your referrer. If you have worsening symptoms or serious concerns, ask your clinician to escalate the review or discuss alternative follow‑up options.
Can Patients Access Imaging Services Without a Referral?
Most NHS imaging requires a GP or specialist referral. Some private providers allow self‑referral, letting patients book directly without a clinician’s recommendation. If you self‑refer privately, make sure your results can be shared with your NHS clinician so care remains integrated.
Conclusion
Understanding how the UK healthcare system organises diagnostic imaging helps patients make informed choices and sets clear expectations for timing and follow‑up. Knowing the roles of NHS structures, Integrated Care Systems and private providers makes it easier to navigate referrals, select appropriate tests and keep care coordinated. Whether you’re using NHS services or exploring private options, clear communication with your clinician and the imaging provider will help you get the right scan at the right time. For more practical guides on accessing diagnostic imaging, explore our resources.
