Pain Management Injection Types & Benefits at Life Medical Imaging
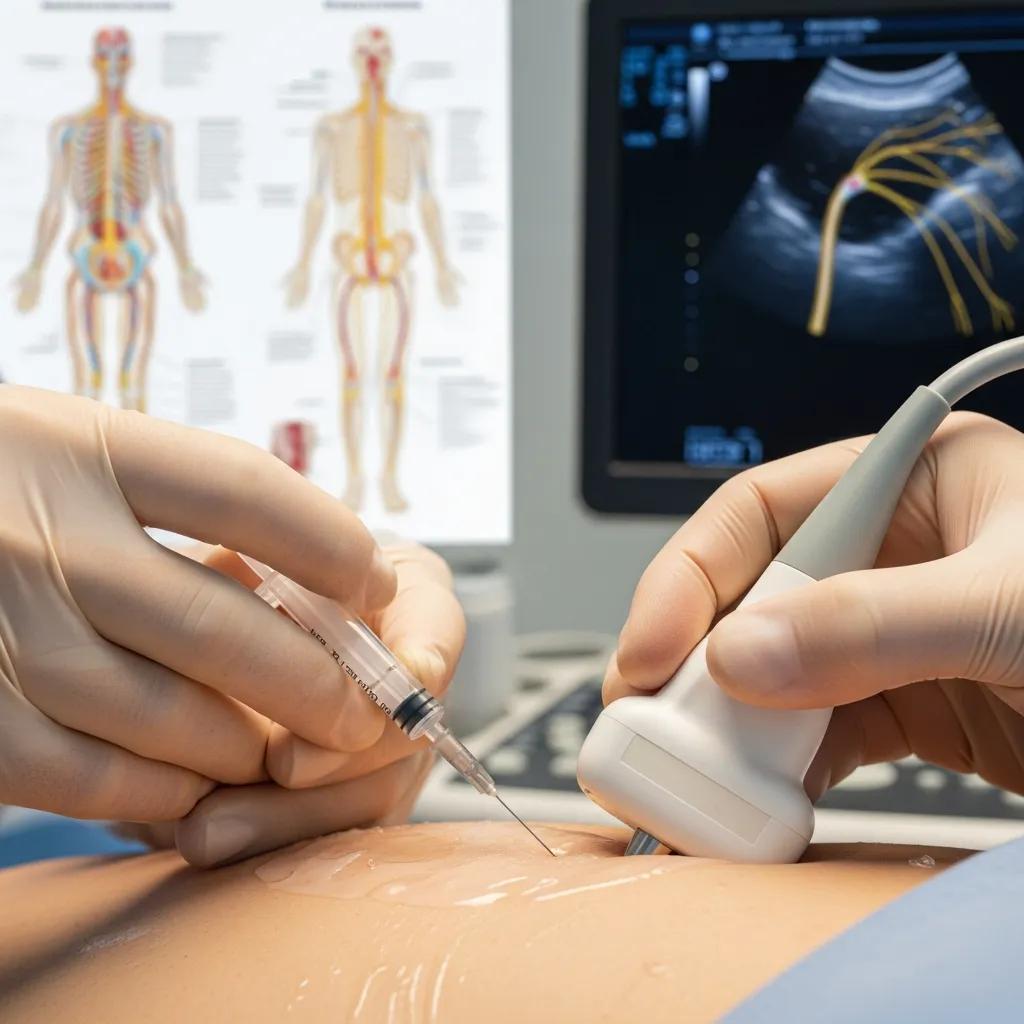
Pain management injections are targeted interventional procedures that place therapeutic medicines directly at the site of pain — into tissues or near nerves — to reduce inflammation, interrupt pain signals and restore function. Common procedures include spinal injections (for example, epidural steroid and facet joint injections), peripheral and diagnostic nerve blocks, joint injections for osteoarthritis, and regenerative therapies such as platelet‑rich plasma (PRP). By combining agents like corticosteroids, local anaesthetic, hyaluronic acid or a patient’s own platelets with image-guided precision, injections often produce faster symptom relief and create a window for active rehabilitation. This article describes the main injection types, how PRP works, the role of nerve blocks, benefits and risks of spinal injections, the imaging‑guided workflow used on the Central Coast, and how injections compare with oral medicines or surgery. Read on for clear definitions, mechanisms, condition‑specific mappings, procedural steps, safety considerations and practical guidance for patients and referrers seeking targeted pain relief.
What are the main types of pain management injections?
Pain management injections are a set of interventional techniques aimed at a specific pain source using agents chosen for their mode of action and expected outcome. Clinicians commonly use a corticosteroid plus local anaesthetic for anti‑inflammatory and anaesthetic effect, hyaluronic acid for joint lubrication, and PRP for regenerative stimulation. Choice of injection depends on the anatomical target and clinical diagnosis. In practice these procedures can be diagnostic (to identify the pain generator) or therapeutic (to reduce inflammation and improve movement). Understanding the main types helps patients and referrers select the most appropriate option for a given problem.
How do epidural steroid injections work for spinal pain?

Epidural steroid injections deliver corticosteroid and local anaesthetic into the epidural space to calm inflammation around spinal nerve roots and reduce nociceptive signalling. The steroid dampens local inflammatory mediators while the local anaesthetic provides rapid pain relief — which can also help confirm the source of symptoms. Typical indications include sciatica from nerve root irritation, symptoms from a herniated disc and selected cases of spinal stenosis where nerve inflammation is the dominant pain driver. Outcomes vary between patients; many experience short‑ to medium‑term relief that allows more effective physiotherapy and gradual return to activity.
What are joint pain relief injections and when are they used?
Joint injections deposit medication directly into a synovial joint or surrounding structures to reduce pain and improve movement. Common agents are corticosteroids for quick anti‑inflammatory effect, hyaluronic acid for viscosupplementation in osteoarthritis, and PRP for regenerative support in tendon and cartilage disorders. Typical targets include the knee, shoulder, hip and smaller peripheral joints affected by osteoarthritis, bursitis or flare‑ups of inflammation. Expected relief varies with the agent and pathology — from weeks to months — so choosing the right treatment depends on whether the goal is short‑term symptom control, viscosupplementation or regenerative benefit.
These procedures are available through interventional imaging services that use image guidance to improve accuracy and safety. Life Medical Imaging Central Coast offers interventional pain procedures including spinal injections, joint injections and PRP therapy, all performed with imaging support to enhance placement and outcomes.
Use the comparison table below to help patients and referrers weigh options based on condition and typical duration of relief.
This table summarises how each injection type maps to common conditions, typical agents used and the expected duration of symptom improvement. Use it as a starting point for discussion with your referrer or treating clinician.
How does platelet‑rich plasma therapy provide pain relief?
Platelet‑rich plasma (PRP) therapy concentrates a patient’s own platelets to deliver growth factors and cytokines that support tissue repair, reduce harmful inflammation and encourage extracellular matrix remodelling. The key mechanism is platelet‑derived growth factors stimulating local healing pathways, which can lead to reduced pain and improved function over weeks to months. PRP is commonly considered for chronic tendinopathies and selected cases of joint osteoarthritis where regenerative modulation may add benefit alongside structured rehabilitation. Recent studies show positive outcomes in conditions such as lateral epicondylopathy and some knee osteoarthritis cohorts, though evidence strength varies by condition and by PRP preparation method.
What conditions can PRP therapy treat effectively?
PRP is most often used for chronic tendinopathies — for example, tennis elbow, Achilles tendinopathy and degenerative rotator cuff conditions — where the normal healing response is impaired. It is also used selectively for knee osteoarthritis to reduce pain and improve function when conservative measures are insufficient. Evidence is stronger for some tendinopathies than for osteoarthritis, and patient selection is important. Discussing likely outcomes, alternative treatments and a concurrent rehabilitation plan helps set realistic expectations.
What is the procedure and recovery process for PRP injections?
PRP is prepared from a brief blood draw and centrifugation to concentrate platelets; the autologous product is then injected into the target tissue, usually under imaging guidance to confirm accurate placement. On the day, local anaesthetic and guided techniques minimise discomfort; patients are observed briefly before discharge and given tailored post‑procedure advice. Expect a temporary increase in soreness for a few days, then gradual improvement over several weeks. Rehabilitation and activity modification are important to maximise functional gains. Image guidance improves accuracy for tendon and intra‑articular injections and supports safer delivery.
These considerations highlight PRP’s role as a targeted regenerative option used alongside guided rehabilitation and realistic recovery timelines.
What are nerve block injections and how do they help?
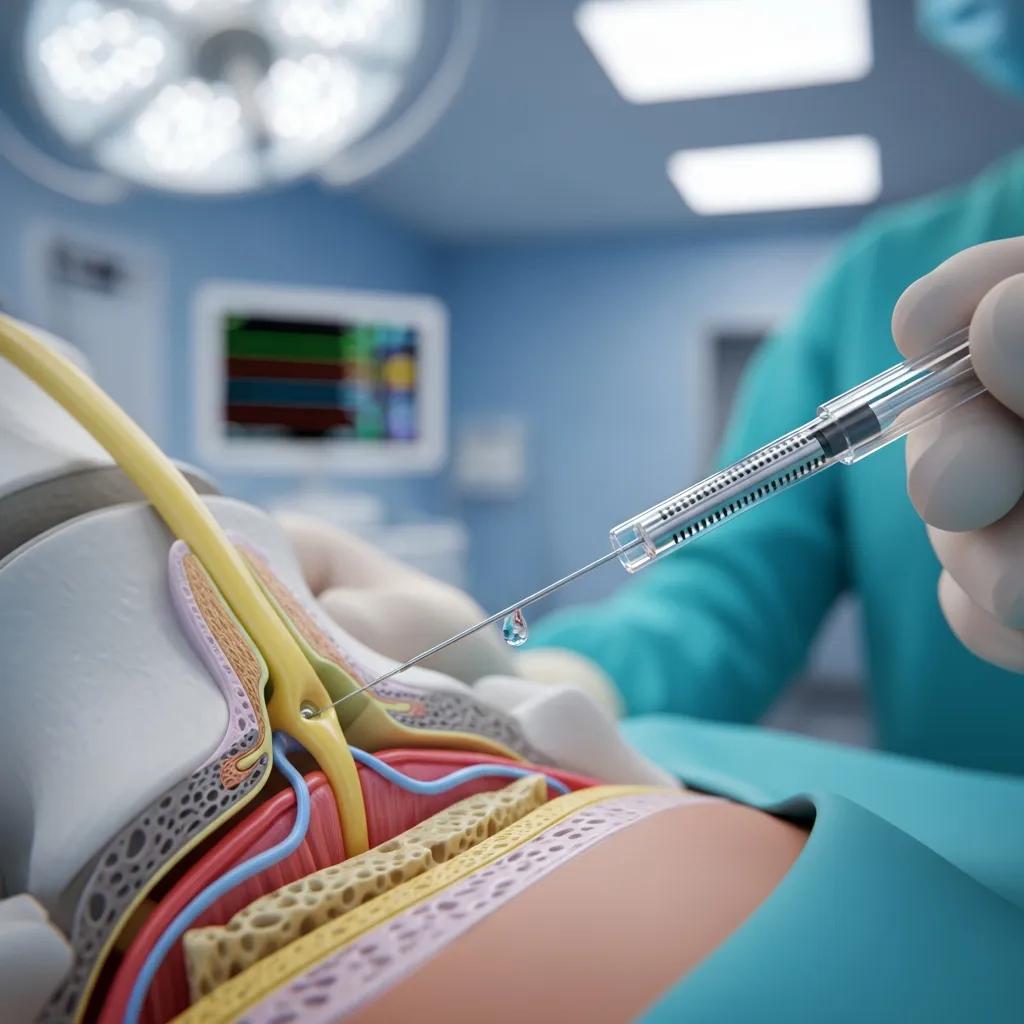
Nerve block injections interrupt pain transmission by delivering local anaesthetic, sometimes with steroid, next to peripheral nerves or nerve roots for diagnostic or therapeutic purposes. Blocks may be peripheral (targeting a named nerve), nerve‑root (targeting a spinal nerve root) or sympathetic (targeting autonomic contributors to pain). They help identify the pain source and can provide immediate symptom control. Therapeutically, nerve blocks can reduce neuropathic or radicular pain, improve sleep and function, and guide further interventions by confirming the pain generator. Real‑time imaging improves accuracy and safety when performing these blocks.
Which conditions are treated with nerve block injections?
Nerve blocks are used for radicular sciatica, certain neuropathic pain syndromes, part of a broader plan for complex regional pain syndrome, and selected chronic regional pain states where targeted nerve interruption relieves symptoms. Diagnostic blocks are particularly valuable when clinical findings and imaging do not align, as they can clarify whether a planned surgical or other intervention is likely to help. Outcomes depend on correct localisation and the underlying pathology; a positive diagnostic block can meaningfully alter the treatment plan. Coordination with referring clinicians ensures blocks fit a wider management strategy.
How are nerve block injections performed with imaging guidance?
Imaging guidance — typically ultrasound for superficial peripheral nerves and fluoroscopy or CT for deeper or spinal nerve root targets — allows clinicians to see anatomy, track needle position and confirm agent spread around the target. Real‑time imaging lowers the risk of intravascular or intraneural injection and increases the chance of a therapeutic effect through precise placement. Patients can expect skin preparation, a short procedure under local anaesthetic and brief post‑procedure observation. Skilled operators and modern imaging technology together reduce complications and improve diagnostic yield.
In short, nerve blocks offer targeted diagnostic and therapeutic options that can rapidly reduce pain and inform longer‑term management decisions.
What are the benefits and risks of spinal pain injections?
Spinal injections can reduce nerve‑root inflammation, provide rapid analgesia, clarify the pain source and enable rehabilitation — and for some patients they can delay or avoid the need for surgery. The primary mechanism is anti‑inflammatory action from corticosteroids combined with temporary local anaesthesia, creating a functional window for physiotherapy. Risks range from common, minor effects to rare but serious complications; understanding both benefits and risks helps patients make informed choices. Using imaging guidance and standardised protocols reduces procedural risk and improves accuracy.
How do spinal injections improve mobility and reduce inflammation?
Spinal injections lower inflammatory mediators around compressed or irritated nerve roots, which diminishes pain signalling and the muscle guarding that restricts movement. The analgesic window provided by the injection often allows patients to engage in physiotherapy and graded activity, producing functional gains that can outlast the pharmacologic effect. Improvements typically begin within days to weeks and may continue for several months, depending on the underlying pathology and adjunctive rehabilitation. Not every patient responds; setting realistic expectations and combining therapies optimises outcomes.
What are the potential side effects and safety considerations?
Common immediate effects include transient local soreness, short‑lived numbness or light‑headedness, and occasional steroid‑related systemic effects such as temporary hyperglycaemia in susceptible patients. Less common but more serious risks include infection, bleeding or nerve injury; these complications are rare when procedures are performed under sterile conditions with appropriate imaging. Pre‑procedure screening, informed consent and careful medication review (including anticoagulant management) are essential risk‑mitigation steps. Image‑guided placement and experienced clinical teams further reduce complication rates and improve safety profiles.
Below is a focused comparison of benefits and risks, and how imaging guidance affects each aspect to support clinical decision‑making.
This comparison clarifies where benefits concentrate and where risks occur, emphasising the role of imaging guidance in reducing adverse events and improving therapeutic targeting.
How are pain management injections guided and administered at Life Medical Imaging Central Coast?
Image‑guided injection workflows combine diagnostic imaging, sterile technique and clinical expertise to place agents precisely where they are needed, with the aim of maximising benefit and reducing complications. At our NATA‑accredited independent radiology clinic on the Central Coast, interventional pain procedures use the imaging modality best suited to the anatomy and clinical question. The typical patient pathway includes referral review, pre‑procedure screening and consent, the image‑guided injection performed by experienced clinicians, and brief post‑procedure monitoring with follow‑up recommendations. This structured pathway supports safe, patient‑centred care in a professional environment.
What imaging technologies are used for accurate injection placement?
Different imaging modalities suit different targets: ultrasound gives real‑time soft‑tissue visualisation for peripheral joint injections and superficial nerve blocks; fluoroscopy provides real‑time bony landmarks for spinal procedures such as epidurals and facet injections; and CT is used selectively for deep or complex anatomy requiring cross‑sectional detail. Each modality offers benefits: ultrasound avoids ionising radiation and provides dynamic needle visualisation; fluoroscopy is fast and reliable for skeletal landmarks; CT gives high‑resolution localisation for difficult targets. Clinicians choose the modality that best balances image clarity, target depth and patient safety for each case.
The table below maps common imaging modalities to their primary uses, advantages and what patients can expect.
This table explains modality selection and sets realistic expectations for patients considering image‑guided injections.
Life Medical Imaging Central Coast provides these interventional imaging options within its Interventional Procedures Pain Management service, supported by modern equipment, skilled clinical and support staff, and a patient‑centred approach. Patients and referrers can request image‑guided spinal injections, joint injections or PRP therapy through standard referral pathways; when booking, ask the referrer to include relevant clinical notes and any available imaging to streamline pre‑procedure planning. The clinic’s accreditation and structured workflow provide reassurance about procedural quality and team expertise.
What should patients expect before, during and after their injection?
Before the procedure patients undergo referral review, medication reconciliation and informed consent to confirm suitability and safety; clear pre‑procedure instructions are provided to optimise outcomes. During the procedure the skin is prepared, local anaesthetic is used and imaging guidance helps position the needle precisely before the therapeutic agent is delivered. After the injection patients receive specific aftercare advice including activity modification, what soreness to expect and when to resume exercise or seek urgent review for concerning signs. Follow‑up with the referrer or the imaging service is recommended to assess response and plan any further rehabilitation or interventions.
This stepwise patient journey sets clear expectations, reduces anxiety and supports a safe recovery that benefits from imaging‑guided accuracy.
How do pain management injections compare with other pain relief treatments?
Pain management injections are targeted interventions that often provide faster symptom relief than oral medicines and carry lower immediate morbidity than surgery for selected indications, though their effects can be temporary and variable. Injections are commonly used as a bridge to rehabilitation, as diagnostic tools to confirm pain generators, and sometimes as definitive therapy when conservative measures fail. The decision to use injections depends on symptom severity, imaging‑confirmed pathology, the response to prior conservative care and overall treatment goals. Comparing injections with oral medicines, physiotherapy and surgery requires weighing duration of effect, systemic side effects, invasiveness and the patient’s functional aims.
- Targeted injections are preferred when oral medicines are insufficient and imaging suggests a discrete pain generator.
- Injections can enable rehabilitation by reducing pain and improving mobility, allowing active recovery.
- Surgery remains appropriate when structural pathology requires repair; injections are not a substitute for needed operative correction.
When are injections preferred over oral medications or surgery?
Injections are typically considered after conservative measures — such as physiotherapy and simple analgesics — have not provided adequate relief, or when diagnostic clarity is needed to localise the pain source. They are also chosen to reduce systemic medication exposure, provide rapid functional improvement and create a window for active rehabilitation. Where structural failure requires operative correction, injections may be adjunctive rather than curative, so an informed discussion about likely outcomes is important. Shared decision‑making between patient and referrer ensures injections are used where they offer the greatest net benefit.
What are the advantages of minimally invasive pain relief procedures?
Minimally invasive injections deliver targeted therapy with lower immediate complication rates and shorter recovery than open surgery. They are often day procedures performed under image guidance to maximise safety, reduce reliance on systemic medicines and provide diagnostic clarity when used as blocks. In many cases they enable meaningful functional improvements that support rehabilitation. Limitations include variable duration of benefit and a proportion of patients who do not achieve meaningful relief, requiring alternative strategies. Overall, injections are a valuable part of a multimodal pain management pathway when matched appropriately to pathology and patient goals.
To arrange a consultation, request an appointment or contact the imaging service, use the standard referral channels and include clear clinical information and any available imaging. Life Medical Imaging Central Coast accepts referrals for Interventional Procedures Pain Management — including spinal injections, joint injections and PRP therapy — and our NATA accreditation, up‑to‑date imaging technology and experienced staff support a patient‑centred, image‑guided care pathway.
- Next step for patients: Ask your referrer to include a brief clinical history and the suspected target when requesting a pain injection appointment.
- Next step for referrers: Specify the intended procedure and attach any relevant imaging to streamline pre‑procedure planning.
- Booking reminder: Use the clinic’s standard referral process to request an appointment or an interventional consultation.
Frequently asked questions
What is the typical recovery time after a pain management injection?
Recovery varies with the injection type and the individual. Most people have some soreness at the injection site for a few days. Many can resume normal daily activities within a day or two, though avoiding strenuous activity for about a week is commonly advised. Follow‑up appointments help assess the injection’s effect and plan any further rehabilitation.
Are pain management injections safe for everyone?
While injections are generally safe, they are not suitable for everyone. Medical conditions, drug allergies or the use of anticoagulant medications can affect eligibility. Discuss your medical history and concerns with your healthcare provider to determine suitability. Informed consent is an important step to ensure patients understand the risks and benefits.
How long do the effects of pain management injections last?
Duration of relief varies by injection type and condition. Corticosteroid injections often give relief for weeks to months; PRP may take longer to produce benefit but can last for several months. Individual responses differ, so it’s important to discuss expected outcomes with your clinician to set realistic goals.
Can pain management injections be repeated?
Yes — many injections can be repeated, but frequency depends on the procedure and the patient’s condition. For example, corticosteroid injections are usually spaced by a few months, while PRP courses may be spaced further apart. Repeat dosing decisions should follow assessment of response and any side effects, with regular follow‑up consultations guiding timing.
What should I do if I experience side effects after an injection?
If you notice increased pain, swelling, fever, redness or any concerning symptoms after an injection, contact your healthcare provider promptly. Most side effects are mild and short‑lived, but early communication allows timely assessment and management of any serious complications.
How do I prepare for a pain management injection?
Preparation typically includes informing your provider about all medications (especially blood thinners), allergies and medical conditions. Follow any fasting or medication instructions given by the clinic. If sedation is planned, arrange for someone to drive you home. Adhering to the pre‑procedure instructions you receive helps ensure a smooth and safe experience.
Conclusion
Pain management injections deliver targeted therapy directly to the source of pain, helping to reduce inflammation, restore movement and create a practical window for rehabilitation. Understanding the range of options — from epidural steroid injections and joint injections to PRP and nerve blocks — lets patients and referrers make informed choices tailored to the condition and treatment goals. When selected appropriately and performed with image guidance by experienced teams, injections can significantly improve quality of life and function. If you’re considering image‑guided pain relief, speak with your referrer about a consultation to explore the most suitable plan for your needs.