AI-Enhanced Imaging: Precise Diagnosis & Care at Life Medical Imaging
Medical imaging AI describes software that uses machine learning and deep learning to review radiology images, highlight patterns and present measurable findings for radiologists and treating clinicians. These systems are trained on large sets of labelled images so they learn to recognise features—such as nodules, haemorrhage or vessel narrowing—and then flag or measure those findings to speed diagnosis and reduce missed abnormalities. This article explains what medical imaging AI is, the core technologies behind it, how it improves accuracy and workflow across CT, MRI, ultrasound and X‑ray, and the safety and ethical safeguards in place. We also outline practical benefits for patients and referring doctors, and explain how to book AI‑enhanced imaging on the Central Coast. Throughout, our aim is a clear, patient‑friendly explanation of AI in radiology, clinical use cases, validation considerations and how AI integration affects outcomes and access to services.
What Is Medical Imaging AI and How Does It Work?
Medical imaging AI is software that analyses image data with trained models to support clinical interpretation, detect abnormalities and quantify disease. At its core are pattern‑recognition methods—most commonly convolutional neural networks (CNNs) and other deep learning architectures—that process pixels, segment structures and generate candidate findings for a radiologist to review. The main benefits are faster detection of critical findings and more consistent measurements, which support earlier treatment decisions and better monitoring. Knowing how these systems work explains why AI is being used across CT, MRI, ultrasound and digital X‑ray, and why clinical validation plus human oversight are essential for safe use.
CNNs in Medical Image Analysis: State‑of‑the‑Art and Applications
Convolutional neural networks (CNNs) have delivered strong results across many medical imaging tasks, enabling automated detection, segmentation and classification of pathologies. This review summarises commonly used CNN architectures (for example LeNet, AlexNet, VGGNet, GoogLeNet and ResNet), how they are adapted for clinical images, and their applications across X‑ray, CT, MRI and ultrasound for detection, segmentation and image enhancement.
Convolutional neural networks for medical image analysis: state‑of‑the‑art, comparisons, improvement and perspectives, H Yu, 2021
How Does Artificial Intelligence Enhance Diagnostic Imaging?
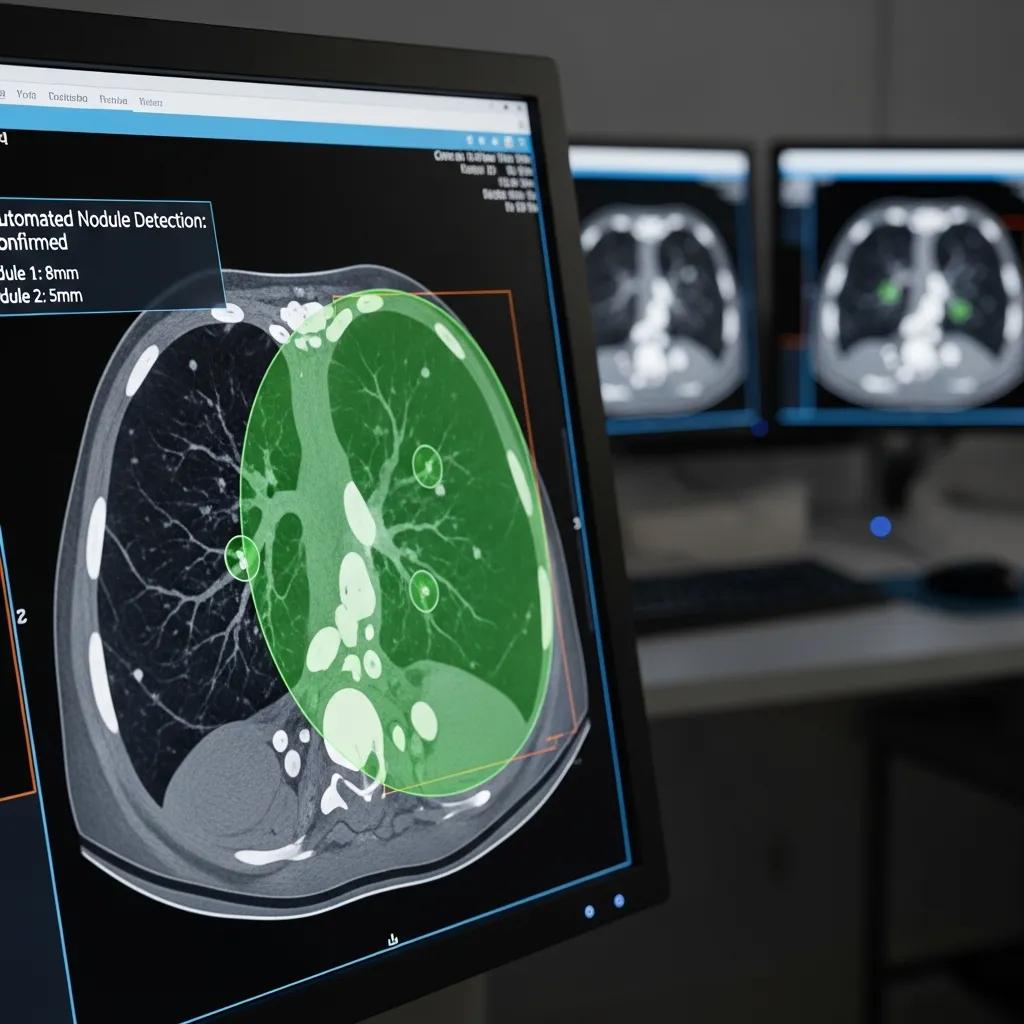
AI strengthens diagnostic imaging by increasing detection sensitivity, automating routine measurements and prioritising likely urgent studies for earlier review. For example, automated nodule detection raises the chance of finding small lung lesions sooner, while segmentation tools provide repeatable tumour volume measurements for treatment planning. Recent studies (2023–2024) report gains in detection rates and shorter time‑to‑report for some acute conditions, reinforcing AI’s value as an assistive tool. Those improvements support faster triage and clearer longitudinal tracking, which together shorten time to treatment and boost clinicians’ confidence in imaging metrics.
What Are the Key Technologies Behind Medical Imaging AI?
Key technologies include supervised machine learning, deep learning (notably CNNs), image pre‑processing pipelines, segmentation modules and post‑processing reporting assistants. Development relies on annotated datasets, data augmentation, cross‑validation and holdout testing to estimate real‑world performance. Clinical validation typically compares AI outputs with radiologist consensus or clinical outcomes. Regulatory and quality frameworks expect human‑in‑the‑loop workflows so radiologists verify AI suggestions; that combination of validated models plus clinician oversight ensures AI augments — not replaces — diagnostic judgement. Understanding these building blocks helps clinicians and patients evaluate claims about accuracy and applicability.
AI and Deep Learning in Medical Imaging: A CNN‑Focused Review
Deep learning and advances in computer vision have unlocked large opportunities for medical image analysis. Research on convolutional neural networks emphasises their ability to capture spatial relationships and hierarchical features through convolution, pooling and backpropagation. Much of the literature focuses on image pre‑processing, classification and practical applications of CNN techniques across clinical imaging tasks.
Convolutional neural network in medical image analysis: a review, D Singh, 2023
How Does AI Improve Diagnostic Accuracy and Efficiency in Radiology?
AI improves accuracy and efficiency by reducing missed findings, standardising quantitative measures and speeding report turnaround. Automated detection increases sensitivity for well‑defined tasks (for example pulmonary nodule detection or intracranial bleed alerts), while reporting assistants pre‑fill measurements and structured text to shorten report drafting. Together these features enable faster clinical decisions and clearer longitudinal comparisons for monitoring disease. The next section outlines the specific mechanisms that produce these benefits and how workflow integration increases their impact.
Before the comparison table, here are core benefits summarised in a quick list that clarifies where AI typically adds value:
- Faster detection of critical findings: AI triage highlights urgent studies for immediate review.
- Improved measurement consistency: Automated segmentation delivers repeatable metrics for follow‑up.
- Reduced reporting times: Auto‑filled measurements and suggested wording speed final reports.
These capabilities free radiologists to focus on complex interpretation and multidisciplinary care.
Different AI functions influence speed, accuracy and workflow in distinct ways; the table below compares those impacts across common attributes.
In What Ways Does AI Enable Faster and More Accurate Diagnoses?
AI speeds diagnosis by prioritising studies likely to contain urgent findings and by supplying immediate quantitative data clinicians can act on. In acute settings—such as stroke or suspected intracranial haemorrhage—triage models can reduce time‑to‑notification and enable quicker escalation. For chronic conditions, AI‑derived measures (for example lesion volume or coronary plaque scoring) create objective baselines that improve monitoring. These mechanisms reduce inter‑reader variability and provide earlier, actionable information for treating teams, shortening the time between imaging and definitive treatment.
How Does AI Optimise Radiology Workflow and Reporting?
AI integrates with PACS/RIS systems to build prioritised reading queues, auto‑populate measurements and suggest structured reporting language for radiologists to verify. This human‑in‑the‑loop approach keeps clinical oversight while removing repetitive tasks, improving throughput without compromising quality. For referrers, clearer structured reports with standardised measurements make decision‑making simpler and reduce the need for clarification. As AI tools mature, they move from novelty to everyday process optimisation, letting radiology teams spend more time on complex cases and multidisciplinary coordination.
Which Medical Imaging Modalities Use AI for Enhanced Diagnostics?
AI is used across CT, MRI, ultrasound, digital X‑ray and DEXA, with models tailored to each modality’s imaging physics and clinical tasks. In CT, AI helps with reconstruction and denoising for low‑dose protocols and assists cardiac/angiography tasks; MRI benefits from faster acquisition and contrast‑free reconstruction algorithms for patients with contrast contraindications. Ultrasound gains automated measurements and view classification, while X‑ray AI speeds triage and nodule screening. The table below maps modalities to common AI applications and the clinical benefits you can expect.
How Is AI Applied in CT Scans and Low‑Dose Imaging?
In CT, AI supports iterative reconstruction and advanced denoising that preserve image quality from lower radiation doses, enabling ultra‑low‑dose protocols while maintaining diagnostic detail. For cardiac CT and angiography, AI assists vessel segmentation, plaque characterisation and automatic calcium scoring to streamline assessments. These tools help radiologists obtain the required diagnostic information with less exposure and faster post‑processing, improving patient safety and throughput. When combined with task‑specific detection models, CT workflows gain sensitivity while reducing radiation burden.
What Are the Benefits of AI in MRI and Contrast‑Free Imaging?
AI accelerates MRI by reconstructing full‑resolution images from undersampled acquisitions and by enabling techniques that shorten scan times. Contrast‑free AI methods can highlight tissue characteristics that previously required gadolinium, providing safer alternatives for patients with renal impairment or other contraindications. The outcomes are shorter appointments, more scanner capacity and safer options for vulnerable patients. These advances also help broaden access to diagnostic MRI through more efficient protocols that meet clinical demand.
How Does AI Assist Ultrasound and Digital X‑ray Analysis?
In ultrasound, AI automates measurements (for example fetal biometry or carotid intima‑media thickness), classifies views and detects common pathologies to reduce operator dependence and reporting variability. For digital X‑ray, AI algorithms can screen for nodules, fractures and other patterns to prioritise worklists and prompt timely follow‑up. While AI can speed initial interpretation, final clinical decisions rely on radiologist verification and correlation with the clinical history. These tools improve consistency and help sonographers and radiographers deliver standardised baseline data for radiologist review.
How Does Medical Imaging AI Benefit Patients and Referring Doctors?
Medical imaging AI provides clear benefits for patients and the clinicians who refer them: faster results, more reliable measurements and better communication between imaging and treatment teams. Patients can experience quicker reporting and—on some exams—lower radiation or contrast exposure. Referrers receive more actionable reports and priority notifications for urgent findings. The table below links stakeholders to AI features and practical outcomes so both patients and clinicians can see where AI adds value.
Locally, Life Medical Imaging Central Coast embeds AI‑enhanced workflows across its diagnostic services on the Central Coast (Bateau Bay; Killarney Vale; Umina Beach; Erina). Patients can expect faster preliminary triage and consistent quantitative reporting where AI assists analysis, with all AI outputs reviewed by specialist radiologists as part of routine practice. For appointments or enquiries about AI‑assisted scans, patients and referrers may phone 02 4326 7000 or use the site’s booking options labelled “Request an Appointment” or “Book Online” to arrange imaging at a convenient Central Coast location.
What Are the Patient Advantages of AI‑Enhanced Imaging?
For patients, the main benefits are speed, safety and clearer measurements. Faster triage shortens time to clinical decisions; denoising and advanced reconstruction reduce radiation exposure in CT; and contrast‑free MRI options lower risks for those who cannot receive contrast. AI‑derived quantitative measures also mean follow‑up comparisons use consistent metrics, improving confidence when monitoring disease. Patients should expect that AI outputs are reviewed by radiologists so any automated finding is checked and placed into the correct clinical context.
How Does AI Support Referring Doctors in Clinical Decision‑Making?
For referring clinicians, AI provides objective metrics, standardised reports and priority alerts that make imaging information clearer and timelier. Objective measurements—such as lesion volumes or calcium scores—help guide treatment decisions and enable better tracking of progression or response. Priority alerts speed communication for urgent cases, supporting faster referrals to specialist care or emergency treatment. These features reduce uncertainty and allow more proactive patient management based on reliable imaging data.
What Are the Latest Advances and Safety Measures in AI Medical Imaging?
Recent advances (2023–2024) include better automation for prostate MRI interpretation, stroke triage models that shorten time to thrombolysis decisions, and reconstruction methods that enable contrast‑free MRI sequences. At the same time, safety measures focus on rigorous validation, human‑in‑the‑loop reporting models and adherence to accreditation frameworks to ensure consistent quality. Responsible deployment emphasises clinical trials, prospective validation and ongoing quality assurance so AI improves care without introducing unintended risk. The next section explains how local clinics follow ethical and safety best practice.
Ethical Considerations for AI in Radiology: Navigating Risks and Patient Protection
AI has major potential to accelerate medical discovery and transform healthcare. In radiology, however, implementation brings challenges that must be managed carefully. This review discusses the risks and ethical issues of clinical AI—such as patient protection, transparency and bias—and highlights the need to implement AI in ways that uphold established ethical and legal standards while protecting patient interests.
Ethical considerations for artificial intelligence: an overview of the current radiology landscape, TA D’Antonoli, 2020
How Does Life Medical Imaging Central Coast Ensure Ethical and Safe AI Use?
Life Medical Imaging Central Coast applies AI responsibly by keeping radiologist oversight on all AI outputs and using validated tools within standard reporting workflows, consistent with NATA‑accredited quality systems. AI outputs are treated as decision‑support information rather than final diagnoses; radiologists verify, contextualise and sign reports to reflect comprehensive clinical judgement. Patients can discuss any concerns about AI interpretation with the reporting clinician or imaging team. For questions or to arrange imaging, patients and referrers may contact the practice by phone at 02 4326 7000 or use the booking prompts labelled “Request an Appointment” or “Book Online” to start the process.
What Recent Research Supports AI’s Role in Medical Imaging?
Peer‑reviewed studies from 2023–2024 highlight AI gains in focused tasks such as automated prostate lesion detection on MRI, rapid CT triage for stroke and improved nodule detection on chest imaging, often showing higher sensitivity or faster reporting in controlled settings. Prospective validation studies also report workflow benefits in emergency departments where AI prioritisation reduced time‑to‑notification. While the evidence base is growing, a consistent finding is that AI performs best when narrowly focused on well‑defined tasks and when used together with radiologist review—supporting a human‑in‑the‑loop model that balances automation and clinical oversight.
How Can Patients Book AI‑Enhanced Medical Imaging Services?
Booking an AI‑enhanced diagnostic scan follows the same basic steps as other specialist imaging, but patients should note referral requirements and any preparation that helps obtain images suitable for AI analysis. Clinics usually require a referring letter or electronic referral from a GP or specialist, and they provide pre‑scan instructions (for example fasting for certain tests). The numbered list below shows a simple booking pathway patients can follow to prepare for AI‑assisted imaging.
- Obtain a referral from your GP or specialist that specifies the modality and clinical question.
- Contact the imaging centre by phone or use the website booking options labelled “Request an Appointment” or “Book Online” to choose a convenient site and time.
- Follow the clinic’s pre‑scan instructions, and bring your referral and any previous imaging for comparison.
This process helps the imaging team acquire the right study and clinical information so AI tools can provide the most useful assistance during analysis.
To make practical preparation easy, here is a short checklist to review before your appointment:
- Bring your referral and any prior imaging reports.
- Confirm preparation instructions (for example fasting or medication guidance).
- Arrive a little early to complete registration and consent paperwork.
These simple steps help ensure high‑quality images and a smooth visit. The next section answers common questions patients have about AI in imaging.
What Is the Process to Book an AI‑Driven Diagnostic Scan?
Booking an AI‑assisted scan begins with a clinician referral, then proceeds through scheduling and pre‑scan preparation much like a conventional imaging appointment. After referral, patients can phone the imaging centre or use online booking prompts to select a Central Coast site and a suitable appointment. The centre provides pre‑scan instructions based on the modality; on the day, technologists follow validated acquisition protocols, AI algorithms may run during post‑processing, and all findings are reviewed and finalised by a radiologist. This staged approach balances efficiency with clinical oversight to deliver accurate, meaningful results.
What FAQs Should Patients Know About AI in Their Medical Imaging?
Common patient questions include whether AI will replace radiologists, how personal data is handled, and how accurate AI is. AI is an assistive technology that supports radiologists — it does not replace clinical judgement — and all AI outputs at accredited clinics are reviewed by specialist radiologists. Clinics use quality assurance processes and follow accreditation standards to protect data and validate performance. Accuracy varies by task and is strongest for narrowly defined detection or measurement jobs; if you have concerns, discuss them with the imaging team when booking or at your appointment.
- Will AI replace the radiologist? No. AI assists radiologists by automating routine tasks and highlighting findings, but final interpretation remains the radiologist’s responsibility.
- Is my data safe? Yes. Imaging services operating under accreditation frameworks implement data governance and secure handling of medical records as standard practice.
- How accurate is AI? It depends on the task. Validation studies show improved detection or efficiency for many targeted applications when used with radiologist oversight.
Frequently Asked Questions
What are the potential risks associated with AI in medical imaging?
AI offers significant benefits but does carry potential risks. Over‑reliance on AI without proper validation or oversight could lead to missed findings. There are also data privacy and security concerns since sensitive health information is processed. Robust validation, ongoing quality assurance and maintained human oversight are essential to reduce these risks and keep patient trust.
How does AI impact the training of radiologists?
AI is changing radiology training by automating routine tasks and creating opportunities to concentrate on complex cases and clinical decision‑making. Training programmes increasingly include AI tools so future radiologists learn to use these systems effectively while preserving core interpretive skills and clinical judgement.
What ethical considerations are involved in using AI for medical imaging?
Key ethical issues include informed consent, data privacy, transparency about how algorithms work and monitoring for bias. Patients should be informed about how their data are used, and AI outputs must be treated as supportive information rather than definitive diagnoses. Ongoing ethical oversight and clear governance frameworks are important to manage these concerns responsibly.
How can patients ensure they receive the best care with AI‑enhanced imaging?
Patients can get the best care by asking their healthcare team how AI is used in their imaging, who reviews the results, and what measures protect their data. Understanding the benefits and limits of AI helps patients make informed choices. Open conversation with clinicians fosters trust and clearer decision‑making.
What should patients do if they have concerns about AI in their imaging results?
If you have concerns about AI in your imaging, raise them with your radiologist or referring clinician. They can explain how AI was used in the analysis, how results were reviewed and what the findings mean for your care. Radiologists are available to discuss interpretation and answer questions to ensure you feel informed and supported.
Are there specific conditions where AI has shown significant improvements in diagnostic accuracy?
Yes. AI has shown notable improvements in tasks such as detecting pulmonary nodules, identifying intracranial haemorrhages and spotting prostate lesions on MRI. Studies indicate AI can enhance sensitivity and reduce missed findings in these focused areas, leading to earlier, more accurate diagnoses. Integrating AI into workflows supports more consistent measurements and faster reporting, benefiting patient outcomes and treatment timelines.
Conclusion
Medical imaging AI can improve diagnostic accuracy and efficiency by detecting critical findings sooner and producing more consistent measurements. By applying validated AI across modalities, patients benefit from quicker results and, in some cases, reduced exposure to radiation or contrast. Referring doctors receive clearer, actionable reports that help guide timely clinical decisions, ultimately improving patient care. To experience the advantages of AI‑enhanced imaging, consider booking an appointment with Life Medical Imaging Central Coast.

